Duke Heart Pulse – week ending May 29th 2022
Memorial Day
This has been a difficult week for our country as we continue to struggle with the pattern of senseless gun violence and the safety of our communities. On behalf of the Duke Heart Leadership team, we’d like to wish all of you a very safe and peaceful Memorial Day weekend. As our nation takes time to remember all those who have been lost while serving in the U.S. military, we hope you’re able to spend some time in self-care, in reflection, and hopefully in the company of those most dear to you. Thank you for all that you do to make Duke Heart one of the very best places to work and care for others.
Duke Execs Kick-off Heart Walk Season
Cardiologist Rick Shannon, MD, Chief Quality Officer for Duke Health, is serving as the Triangle-area campaign chair for the 2022 Triangle Heart Walk. He recently hosted two Heart Walk kick-off events for senior leaders across Duke University Health System. The first was held May 12 at Duke University Hospital and the second was held on Thursday morning at Duke Raleigh.
Duke Heart’s leadership team shared highlights and successes of our ongoing partnership with the American Heart Association (AHA) both locally and nationally, as well as personal accounts of why supporting fundraising efforts like the Heart Walk are important. Cardiovascular disease and stroke have impacted most members of our team in some way — and hearing team members share their “why” stories and our efforts toward research, care and prevention was deeply inspiring.
We’re looking forward to a successful Heart Walk this fall–be on the lookout for more information. We’d like to make this our biggest and most successful year, ever! The date of the walk will be announced this summer.
Speaking of our AHA partnership, congratulations to our colleagues in the Duke Stroke Center! Two of their teams from Duke Raleigh Hospital participated in the Triangle CycleNation event held by the AHA on May 17 at Coastal Credit Union Midtown Park at North Hills in Raleigh. The teams raised funds to help fight stroke and increase awareness around stroke prevention and warning signs. Good work!




Highlights: AATS 2022
The American Association for Thoracic Surgery (AATS) 102nd annual meeting took place the weekend of May 14-17 in Boston.
Duke highlights included:
Presentations by thoracic surgeons Betty Tong and Matt Hartwig – they were each recognized during AATS 2022 with separate news briefs in the AATS Daily News on Monday, May 16 .

Tong was highlighted for her AATS presentation, “Lung Cancer Screening in 2022” which she gave on Saturday, May 14. Tong discussed study findings that demonstrate roughly five percent of screen-eligible patients are getting low-dose computed tomography (LDCT) scans of their chest to screen for lung cancer. Fairly recently, the U.S. Preventative Services Taskforce expanded screening guidelines that make an even larger number of patients screen-eligible, but Tong says, “only time will tell if more people get LDCT scans.” In her interview with AATS Daily News, Tong stated, “Adherence to screening guidelines and follow-up is suboptimal right now.” She discussed accessibility, budget constraints, socio-economic issues and general misconceptions about lung cancer screenings as issues that all contribute to low screening rates. See story on p. 4: https://duke.is/855sp.
Hartwig was highlighted to preview his presentation on proposals for an AATS

consensus document, “The Use of Mechanical Circulatory Support (MCS) for Lung Transplantation” which took place on Monday, May 16. “The AATS believes it’s important to provide the latest
guidance on how to best use modern MCS to benefit our patients before, during, and after lung transplantation,” Hartwig says in the piece. “Establishing an expert consensus document would be the most appropriate way to meet our needs.” See story on p. 6: https://duke.is/855sp.
Jacob Schroder presented the AATS consensus statement on DCD heart transplantation,

“Cardiac Transplantation Utilizing Donors Following Circulatory Death” on Saturday evening, May 15. The consensus statement will soon be published in the Journal of Thoracic and Cardiovascular Surgery; Schroder and Carmelo Milano are the first and senior authors.
Early EXACT Trial Findings Presented as AATS Late Breaker
The Epicardial Delivery of XC001 Gene Therapy for Refractory Angina Coronary Treatment (EXACT) trial is a first-in-human clinical trial examining the safety and efficacy of using an adenoviral vector to more efficiently deliver human vascular endothelial growth factor (VEGF) directly into the myocardium with the goal of stimulating angiogenesis in patients suffering from refractory angina due to advanced coronary artery disease (CAD). Readers may recall the trial launched at Duke last summer when study investigator and cardiothoracic surgeon Adam Williams  performed the first procedure on one of our Duke study participants.
performed the first procedure on one of our Duke study participants.
The preliminary findings in a small sample size of participants suggests a dose-response across several efficacy variables and supports continued investigation in the Phase 2 portion of the trial. Early clinical trial results were presented at AATS by Nahush Mokadam of Ohio State’s Wexner Medical Center, one of the site investigators, on Sunday, May 15.
Additional Duke investigators on the trial include: Tom Povsic, Duke site and national PI, and executive committee member E. Magnus Ohman, who Povsic credits with getting  this study to Duke.
this study to Duke.
- Related EXACT news: Povsic presented the 6-month follow up data “Preliminary Safety, Tolerability and Efficacy of Direct Epicardial Administration of Encoberminogene Rezmadenovec (XC001) to Ischemic Myocardium in Patients with Refractory Angina: Six Month Phase 1 Data for the EXACT Trial” at the American Society of Gene and Cell Therapy

Magnus Ohman in Boston on May 18th.
Additional Duke presenters at AATS included faculty members: Thomas D’Amico, Jacob Klapper, David Harpole, Edward Chen and Chad Hughes, as well as the following members of Duke’s general surgery residency program: Vignesh Raman, Christopher Jensen, Kristen Rhodin and Samuel Kesseli.
Impressive work! Congratulations to all!
NCDR Announces 2022 Chest Pain-MI Awards
 We are excited to share our latest performance achievement awards for the American College of Cardiology’s Chest Pain-MI Registry. This week we were notified by the National Cardiovascular Data Registry (NCRD) of our latest ratings across all three hospitals.
We are excited to share our latest performance achievement awards for the American College of Cardiology’s Chest Pain-MI Registry. This week we were notified by the National Cardiovascular Data Registry (NCRD) of our latest ratings across all three hospitals.
- Duke Regional Hospital: Silver
- Duke Raleigh Hospital: Platinum
- Duke University Hospital: Platinum
More than 2,400 hospitals and over 8,500 outpatient providers worldwide participate in one or more of the ACC’s ten registries, such as Chest Pain-MI, forming a comprehensive network of cardiovascular care providers committed to ensuring evidence-based cardiovascular care, improving patient outcomes and lowering health care costs.
The Chest Pain-MI Registry is the most trusted source for outcomes-based, continuous quality improvement, according to the ACC. It is the go-to registry for hospitals and health systems applying ACC and American Heart Association clinical guideline recommendations.
Congratulations to all!
Shout-out to Haney & Ashley!
We received a terrific note this week from Lisa Clark Pickett, Chief Medical Officer for Duke University Hospital, regarding team members Jack Haney and Ciarra Ashley and wanted to share it with you. Pickett wrote:
“Good Morning, Jack and Ciarra,
While reading comments on our Patient Satisfaction Survey I was just delighted to read this lovely compliment about you and your team. Thank you for your continual dedication to patients, professionalism, and excellence!”
The survey note read: “Dr. Haney and his medical team were awesome! Nurses on the 6 East Floor were very attentive to my needs & took excellent care of me. This was the BEST hospital stay for me.” – a grateful patient
Great job!


Kudos to Loriaux, Pagidipati!
We’re also sharing some warm compliments we received regarding cardiology fellow Dan Loriaux and faculty member Neha Pagidipati via Duke Health’s StarCard feedback system.

 “Dr. Pagidipati is an exceptional doctor. Dr. Dan Loriaux, fellow at Duke, is a remarkable young man. If he continues with cardiology, there is no one better to add to the Duke team. Both (Dan and Neha) are uniquely gifted,” the patient wrote (names are withheld in StarCard).
“Dr. Pagidipati is an exceptional doctor. Dr. Dan Loriaux, fellow at Duke, is a remarkable young man. If he continues with cardiology, there is no one better to add to the Duke team. Both (Dan and Neha) are uniquely gifted,” the patient wrote (names are withheld in StarCard).
Another wrote, “Excellent, compassionate care by Dr. Pagidipati. None better.”
Well done!
Latorre Nominated For Daisy Award
Amanda Latorre, one of our wonderful nurses on 7100, was recently nominated for a Daisy Award for providing compassionate care. She received the nomination from a patient’s daughter. The daughter had been present with her mother for the duration of the hospitalization as she was hesitant to leave and miss out on important information. Amanda put the daughter’s mind at ease with her excellent bedside manner and strong communication skills which allowed the daughter to leave for a night of good rest. Amanda also provided the patient with fresh toiletries and a moisturizing foot massage.
Thank you, Amanda, for the exceptional care you continue to provide for our Heart patients!

COVID-19 Update
All the latest Clinical Operations updates related to COVID can be found at https://covid-19.dukehealth.org. Patient-facing resources on DukeHealth.org can be found here: https://www.dukehealth.org/covid-19-update/resources. Duke University maintains a resource page as well, which can be accessed here: https://coronavirus.duke.edu/updates/for-staff.
Upcoming Events & Opportunities
Cardiology Grand Rounds
May 31: Heart Failure Cardiogenic Shock and the Golden Circle with Vanessa Blumer. 5 p.m., Webex.
Duke-Stanford Cardiovascular Research Symposium
June 27 & 28. The Duke-Stanford Cardiovascular Research Symposium returns to Durham this year and is offered as a hybrid event. This symposium is sponsored by the Edna and Fred L. Mandel, Jr. Foundation.
Registration required. In person: Great Hall, Mary Duke Biddle Trent Semans Center, Durham, NC. For those who wish to attend virtually, the event will offer live-streaming. The link will be emailed prior to the program. Registrants who choose the virtual live-streamed webinar option will be able to obtain CE credit for the course. For more information, contact Christy Darnell.

Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged. Submissions by Noon, Wednesdays, to be considered for weekend inclusion.
Duke Heart in the News:
May 20 — Richard Shannon
Axios
Red states aren’t prepared for a post-Roe baby boom
https://duke.is/v4vqs
May 23 — Jennifer Rymer
tctMD
DISRUPT PAD III: Lithotripsy Prep Linked to Better PAD Patency at 1 Year
https://duke.is/ycwfv
May 24 — Sunil Rao
Healio
SCAI president discusses results of the DIPRA trial
https://duke.is/5n3s8
May 24 — Marat Fudim
Medscape
Paradigm-Challenging Heart Failure Treatment Strategy Hopeful in Early Trial
https://duke.is/jze4f
Division of Cardiology Publications Indexed in PubMed May 19-25, 2022
Bier EA, Alenezi F, Lu J, Wang Z, Mammarappallil JG, O’Sullivan-Murphy B, Erkanli A, Driehuys B, Rajagopal S. Noninvasive diagnosis of pulmonary hypertension with hyperpolarised Xe magnetic resonance imaging and spectroscopy. ERJ Open Res 2022 May 16;8(2):00035-2022. PM:35586448.
DeVore AD, Hellkamp AS, Thomas L, Albert NM, Butler J, Patterson JH, Spertus JA, Williams FB, Shen X, Hernandez AF, Fonarow GC. The association of improvement in left ventricular ejection fraction with outcomes in patients with heart failure with reduced ejection fraction: data from CHAMP-HF. Eur J Heart Fail 2022 May;24(5):762-770. PM: 35293088.
Jawitz OK, Lawton JS, Thibault D, O’Brien S, Higgins RSD, Schena S, Vemulapalli S, Thomas KL, Zwischenberger BA. Sex Differences in Coronary Artery Bypass Grafting Techniques: A Society of Thoracic Surgeons Database Analysis. Ann Thorac Surg 2022 Jun;113(6):1979-1988. PM: 34280377.
Kelsey MD, Patrick-Lake B, Abdulai R, Broedl UC, Brown A, Cohn E, Curtis LH, Komelasky C, Mbagwu M, Mensah GA, Mentz RJ, Nyaku A, Omokaro SO, Sewards J, Whitlock K, Zhang X, Bloomfield GS. Inclusion and diversity in clinical trials: Actionable steps to drive lasting change. Contemp Clin Trials 2022 May;116:106740. PM: 35364292.
Kwapong YA, Boakye E, Obisesan OH, Shah LM, Ogunwole SM, Hays AG, Blumenthal RS, Creanga AA, Blaha MJ, Cainzos-Achirica M, Nasir K, Douglas PS, Wang X, Sharma G. Nativity-Related Disparities in Preterm Birth and Cardiovascular Risk in a Multiracial U.S. Cohort. Am J Prev Med 2022 Jun;62(6):885-894. PM: 35597568.
O’Brien EC, Sugarman J, Weinfurt KP, Larson EB, Heagerty PJ, Hernandez AF, Curtis LH. The impact of COVID-19 on pragmatic clinical trials: lessons learned from the NIH Health Care Systems Research Collaboratory. Trials 2022 May 21;23(1):424. PM: 35597988.
Rosenberg P. VDAC2 as a novel target for heart failure: Ca at the sarcomere, mitochondria and SR. Cell Calcium 2022 Jun;104:102586. PM: 35429733.
Saldarriaga C, Atar D, Stebbins A, Lewis BS, Abidin IZ, Blaustein RO, Butler J, Ezekowitz JA, Hernandez AF, Lam CSP, O’Connor CM, Pieske B, Ponikowski P, Roessig L, Voors AA, Anstrom KJ, Armstrong PW. Vericiguat in patients with coronary artery disease and heart failure with reduced ejection fraction. Eur J Heart Fail 2022 May;24(5):782-790. PM: 35239245.
Sata SS, Spratt SE, Edmonston DL, Pagidipati N. Clinical progress note: Indications for and management of sodium-glucose cotransporter-2 (SGLT-2) inhibitors in hospitalized patients. J Hosp Med 2022 May;17(5):360-363. PM: 35535917.
Schocken DD. Registry Evidence for Modulation of the Acute Ischemic Heart Disease Pathway: Statins Prevent Heart Failure? J Am Coll Cardiol 2022 May 24;79(20):2034-2036. PM: 35589165.
Stacey RB, Hall ME, Leaverton PE, Schocken DD, Zgibor J. Relation of glycemic status with unrecognized MI and the subsequent risk of mortality: The Jackson Heart Study. Am J Prev Cardiol 2022 May 10;11:100348. PM: 35600110.
Udell JA, Jones WS, Petrie MC, Harrington J, Anker SD, Bhatt DL, Hernandez AF, Butler J. Sodium Glucose Cotransporter-2 Inhibition for Acute Myocardial Infarction: JACC Review Topic of the Week. J Am Coll Cardiol 2022 May 24;79(20):2058-2068. PM: 35589167.
Duke Heart Pulse week ending May 22nd 2022
Highlights of the week:
Rao Named President of SCAI
 Sunil Rao, MD, professor of medicine in cardiology at Duke and section chief of cardiology at the Durham VA Health System, assumed the office of president of the Society for Cardiovascular Angiography & Interventions (SCAI) on Saturday evening during the SCAI 2022 Scientific Sessions being held May 19-22 in Atlanta, GA. He gave the presidential address.
Sunil Rao, MD, professor of medicine in cardiology at Duke and section chief of cardiology at the Durham VA Health System, assumed the office of president of the Society for Cardiovascular Angiography & Interventions (SCAI) on Saturday evening during the SCAI 2022 Scientific Sessions being held May 19-22 in Atlanta, GA. He gave the presidential address.
Rao graduated summa cum laude from Miami University in Oxford, OH, and magna cum laude from The Ohio State University College of Medicine where he won the David Saylor Memorial Award for cardiology research. He completed a residency in internal medicine and fellowships in cardiology and interventional cardiology at Duke University Medical Center. After his training, he joined the faculty at Duke University Medical Center as an assistant professor of medicine and rose to become professor of medicine in 2017. In 2005, he became the director of the catheterization laboratories at the Durham VA Medical Center, and in 2014, he was appointed chief of cardiology at the Durham VA. Rao has won several awards as an attending physician including the W. Proctor Harvey Award from the American College of Cardiology (2011), and the Duke Cardiology Fellows’ Mentoring Award (2013, 2018), and the DCRI Robert M. Califf MD Award for Fellow Mentoring (2020).
As the VA’s chief of cardiology, Rao has overseen the expansion of the faculty to increase patient access, start new clinical programs, and leverage VA research funding. New clinical programs include a structural heart disease service, a same-day discharge after PCI program, and a transradial PCI program. Under his leadership, the Durham VA is the leading transradial PCI center in the VA system nationally.
In September, Rao will begin a new role as director of interventional cardiology for the NYU Langone Health System in New York. At the national level, Rao serves as Editor-in-Chief of Circulation: Cardiovascular Interventions and is a former chair of the SCAI Quality Improvement Committee and was the program chair for the SCAI 2019 Scientific Sessions.
“It is a tremendous honor to lead SCAI during the next year as we continue to make meaningful progress towards the organization’s priorities outlined in our strategic plan, as well as empower and educate our members who are the leaders of interventional cardiology,” Rao stated. “I look forward to working with our members in the year ahead to improve patient outcomes.”
Congratulations, Sunil!
Additional SCAI Highlights: 
We had several current and former faculty and fellows present and moderate at SCAI. Raj Swaminathan was part of the SCAI program committee and former fellow Amit Vora (now at UPMC) was inducted into the Emerging Leader Mentorship program Congratulations, Raj and Amit!
Jennifer Rymer had two invited oral presentations: Managing bleeding in high risk ACS and Diversifying the Vascular Workforce and panel on cardiogenic shock. Great work, Jenn!

DCRI Fellows Graduation Reception Held
After three years without a formal Duke Clinical Research Institute (DCRI) Fellows’ Graduation Reception, the DCRI team was able to get together in person at the University Club in Durham on Tuesday evening, May 17. There, the team celebrated the accomplishments of nine graduating fellows and wholeheartedly thanked all the mentors and DCRI faculty and staff who supported them.
Graduating trainees from the Heart Center included: Drs. Michelle Kelsey, Andrew Vekstein, Vishal Rao, Vanessa Blumer, and Kelly Arps. The event was attended by several DCRI members/cardiology faculty including Drs. Adrian Hernandez, Manesh Patel, Michael Felker, and Robert Mentz. Several individuals were awarded as follows:
- The DCRI Fellows’ Citizenship Award was given to Andrew Vekstein, MD, resident in the CT Surgery Integrated Thoracic Surgery Residency Program. Mentor: John Alexander.
 The Robert A. Harrington Excellence in Fellowship Award was given to Michelle D. Kelsey, MD. Begun in 2012, this award is designed to recognize a graduating DCRI research fellow who has contributed the most to the DCRI fellowship during his/her tenure and who has demonstrated excellence in academic accomplishments, in participation in clinical research operations, and in peer-to-peer mentoring. Fellows considered for this award are expected to have demonstrated the following key attributes during their DCRI tenure: a passionate pursuit of innovative clinical research, humility, inclusiveness, loyalty to colleagues, consensus-building, and selflessness. All graduating DCRI research fellows are eligible for this award.
The Robert A. Harrington Excellence in Fellowship Award was given to Michelle D. Kelsey, MD. Begun in 2012, this award is designed to recognize a graduating DCRI research fellow who has contributed the most to the DCRI fellowship during his/her tenure and who has demonstrated excellence in academic accomplishments, in participation in clinical research operations, and in peer-to-peer mentoring. Fellows considered for this award are expected to have demonstrated the following key attributes during their DCRI tenure: a passionate pursuit of innovative clinical research, humility, inclusiveness, loyalty to colleagues, consensus-building, and selflessness. All graduating DCRI research fellows are eligible for this award.- The Eric D. Peterson Manuscript Award was given to Vishal N. Rao, MD. Rao won the Peterson award for his JACC
 paper In-Hospital Initiation of Sodium-Glucose Cotransporter-2 Inhibitors for Heart Failure With Reduced Ejection Fraction. This award recognizes a DCRI fellow whose writing excellence is demonstrated in at least one impactful and novel medical article. Through this award, the fellowship program recognizes Dr. Eric D. Peterson, a former DCRI Director, and his contributions to the DCRI fellowship program.
paper In-Hospital Initiation of Sodium-Glucose Cotransporter-2 Inhibitors for Heart Failure With Reduced Ejection Fraction. This award recognizes a DCRI fellow whose writing excellence is demonstrated in at least one impactful and novel medical article. Through this award, the fellowship program recognizes Dr. Eric D. Peterson, a former DCRI Director, and his contributions to the DCRI fellowship program.
In commenting on the event, Sana Al-Khatib, MD, DCRI Fellowship Program Director said, “Congratulations to all the graduating fellows! It was truly wonderful to have the opportunity to celebrate them and to thank everyone who supported them in person. We are very proud of the amazing accomplishments of our trainees and look forward to seeing how they will shape the future and make a difference for patients and the world. We appreciate the tremendous commitment of our faculty and staff who work tirelessly to support our mission to train the next generations.”
Congratulations, Michelle, Andrew, Vishal, Vanessa & Kelly! You are all amazing!



Fudim Presents LBCT at Heart Failure 2022
Marat Fudim, MD, MHS, presented data from the REBALANCE-HF trial this morning (May 22) as part of late-breakers at the Heart Failure 2022 & World Congress on Acute Heart Failure, the annual congress of the Heart Failure Association of the European Society of Cardiology, being held this weekend in Madrid (May 21-24).

The REBALANCE-HF trial is examining the safety and efficacy of a splanchic nerve ablation in patients with heart failure with preserved ejection fraction (HFpEF). Fudim reported on the first 18 patients with HFpEF to have been enrolled into the roll-in, open-label arm of the study. The findings were simultaneously published in the European Journal of Heart Failure.
The preliminary open-label results support the safety and efficacy of splanchnic ablation for volume management (SAVM) in HFpEF. The findings require confirmation in the ongoing randomized, sham-controlled portion of the trial.
In addition to Fudim, Manesh Patel is a co-author. Additional authors from other institutions include Peter S. Fail, Sheldon E. Litwin, Tamaz Shaburishvili, Parag Goyal, Scott Hummel, Barry A. Borlaug, Rajeev C. Mohan, Ravi B. Patel, Sumeet S. Mitter, Liviu Klein, Krishna Rocha-Singh, Vivek Y. Reddy, Daniel Burkhoff and Sanjiv J. Shah.
Congratulations, Marat!
Milano Named Beard Distinguished Professor

Congratulations to Carmelo Milano, MD, professor of surgery in the Division of Cardiovascular and Thoracic Surgery. He has been named the Joseph W. and Dorothy W. Beard Distinguished Professor of Experimental Surgery effective July 1.
Distinguished professorships are awarded to faculty who have demonstrated extraordinary scholarship in advancing science and improving human health. Milano is one of 16 faculty members in the Duke School of Medicine to be awarded a distinguished professorship this year. David Harpole is another; his distinguished professorship was mentioned in a Pulse post last month. The SOM officially announced all professorship on May 19.
To read about each of the 2022 distinguished professorships, please visit: https://medschool.duke.edu/news/meet-school-medicines-2022-distinguished-professors.
Congratulations, Carmelo!
Kelsey on CV Prevention at CGR
Michelle Kelsey presented an engaging cardiology grand rounds on Tuesday, May 17. In CV Prevention: Taking Flight, Kelsey discussed a range of factors impacting cardiovascular disease prevention, including BP guideline variance and too few specialists available to efficiently monitor the 34.2 million people with type 2 diabetes. She stressed the importance of teamwork, comparing it to that of the Wright brothers’ whose partnership made the first successful aircraft flight possible.
Great presentation, Michelle!
2022 FON Excellence Award Winners Celebrated
The 33rd Duke Friends of Nursing (FON) Annual Gala was held last weekend at the Durham Convention Center. Thirty-seven Duke nurses were recognized with Excellence Awards; all 216 nominees and the contributions of Duke nurses across Duke University Health System were celebrated. Each winner was recognized individually with a Friends of Nursing pin, a certificate, an engraved trophy, and a $1,000 education stipend. To watch a replay of the entire celebration from last weekend, click here.
The following Duke Heart team members were recognized with Excellence Awards:
- Ciarra Ashley
- Jo Nocito
- Gilbert Thomas Rutledge
- Diane M. Sauro
- Dustin Tart
- Mutya Valente
- Melissa Williams
FON was launched in 1988 thanks to the vision of Martha White Blalock and Dan S. Blalock Jr., grateful patients who sought a way to thank the nurses who were caring for them during Martha’s hospitalization at Duke. Following Martha’s death, Dan collaborated with others to establish the Friends of Nursing program. He remained closely involved until his passing in 2017. Through the Daniel S. Blalock Jr. Charitable Foundation, Dan continues to make a difference at Duke.
During the 2022 nomination cycle, FON received nominations across all settings of care, with many nurses receiving multiple submissions. The nominations came from patients and their loved ones, and from other nurses and interprofessional colleagues.
“My sincere thanks to those who nominated a colleague,” said Mary Ann Fuchs, vice president of patient care and system chief nurse executive for Duke University Health System. “When you take the time to submit a nomination, you enhance the person’s sense of purpose and well-being, and you help to build a supportive work culture.”
Friends of Nursing nominations are open year-round. To learn more or to nominate a colleague, please visit: https://dukefriendsofnursing.org/nominate-a-nurse.
Congratulations, Ciarra, Jo, Gilbert, Diane, Dustin, Mutya and Melissa! We are so happy for you!







ICYMI: CardioNerds launches AF Series with Arps as Co-Chair
 Our friends at CardioNerds have launched a new series on Atrial Fibrillation. Duke cardiology fellow Kelly Arps co-chairs the series with Colin Blumenthal, a fellow at the University of Pennsylvania. The series launched this week with episode #208, featuring Larry Jackson.
Our friends at CardioNerds have launched a new series on Atrial Fibrillation. Duke cardiology fellow Kelly Arps co-chairs the series with Colin Blumenthal, a fellow at the University of Pennsylvania. The series launched this week with episode #208, featuring Larry Jackson.  Arps and Blumenthal were joined by Dinu-Valentin Balanescu, rising internal medicine chief resident at Beaumont Hospital, to interview Jackson. The topic is Atrial Fibrillation: Epidemiology, Health Equity, & The Double Paradox with Dr. Larry Jackson. Not to be missed – this will be a terrific series!
Arps and Blumenthal were joined by Dinu-Valentin Balanescu, rising internal medicine chief resident at Beaumont Hospital, to interview Jackson. The topic is Atrial Fibrillation: Epidemiology, Health Equity, & The Double Paradox with Dr. Larry Jackson. Not to be missed – this will be a terrific series!
Great job, Kelly and Larry!
COVID-19 Update
All the latest Clinical Operations updates related to COVID can be found at https://covid-19.dukehealth.org. Patient-facing resources on DukeHealth.org can be found here: https://www.dukehealth.org/covid-19-update/resources. Duke University maintains a resource page as well, which can be accessed here: https://coronavirus.duke.edu/updates/for-staff.
Upcoming Events & Opportunities
Cardiology Grand Rounds
May 24: Global Cardiovascular Health in the Peri-Pandemic Era with Mark Huffman of Washington University School of Medicine. 5 p.m. Webex.
May 31: Heart Failure Cardiogenic Shock and the Golden Circle with Vanessa Blumer. 5 p.m., Webex. (Link not yet available.)
Duke-Stanford Cardiovascular Research Symposium
 June 27 & 28. The Duke-Stanford Cardiovascular Research Symposium returns to Durham this year and is offered as a hybrid event. This symposium is sponsored by the Edna and Fred L. Mandel, Jr. Foundation.
June 27 & 28. The Duke-Stanford Cardiovascular Research Symposium returns to Durham this year and is offered as a hybrid event. This symposium is sponsored by the Edna and Fred L. Mandel, Jr. Foundation.
Registration required. In person: Great Hall, Mary Duke Biddle Trent Semans Center, Durham, NC. For those who wish to attend virtually, the event will offer live-streaming. The link will be emailed prior to the program. Registrants who choose the virtual live-streamed webinar option will be able to obtain CE credit for the course. For more information, contact Christy Darnell.
Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged. Submissions by Noon, Wednesdays, to be considered for weekend inclusion.
Duke Heart in the News:
May 12 — Duke Heart
El Heraldo (Honduras)
Brigada regresa al país para aliviar corazones de personas sin recursos
https://duke.is/jtkus
May 15 — Robert Mentz
CBS Mornings
Spirituality can improve outcomes for patients with heart failure (*clip begins @ 01:52:52)
https://duke.is/ykwk3
May 17 — Salim Idriss
Applied Clinical Trials
The Need For Pediatric Clinical Trials and Data
https://duke.is/468ja
May 19 — Sunil Rao
Medpage Today
Distal Radial Artery PCI Access Doesn’t Hurt the Hand
https://duke.is/gw6wg
May 20 — Kelly Arps and Larry Jackson
CardioNerds (#208)
Atrial Fibrillation: Epidemiology, Health Equity, & The Double Paradox with Dr. Larry Jackson
Division of Cardiology Publications Indexed in PubMed May 12-18, 2022
Asher WB, Terry DS, Gregorio GGA, Kahsai AW, Borgia A, Xie B, Modak A, Zhu Y, Jang W, Govindaraju A, Huang LY, Inoue A, Lambert NA, Gurevich VV, Shi L, Lefkowitz RJ, Blanchard SC, Javitch JA. GPCR-mediated β-arrestin activation deconvoluted with single-molecule precision. Cell 2022 May 12;185(10):1661-1675.e16. PM: 35483373.
Bhatt AS, Fonarow GC, Greene SJ. Prioritizing prevention of de novo and worsening chronic heart failure. Eur J Heart Fail 2022 Apr;24(4):653-656. PM: 35218135.
Campbell MM, Benjamin DK, Mann T, Fist A, Kim H, Edwards L, Rak Z, Brookhart MA, Anstrom K, Moore Z, Tilson EC, Kalu IC, Boutzoukas AE, Moorthy GS, Uthappa D, Scott Z, Weber DJ, Shane AL, Bryant KA, Zimmerman KO. Test-to-Stay After Exposure to SARS-CoV-2 in K-12 Schools. Pediatrics 2022 May 1;149(5):e2021056045. PM: 35437593.
DeFilippis EM, Blumer V, Mentz RJ, Agarwal R, Haythe JH, Kittleson M. In-Hospital Outcomes in Pregnancy After Heart Transplantation. Am J Cardiol 2022 Jun 1;172:68-72. PM: 35331474.
Eiger DS, Smith J, Shi T, Stepniewski TM, Honeycutt C, Boldizsar N, Gardner J, Tsai CF, Nicora C, Moghieb A, Kawakami K, Choi I, Smith R, Inoue A, Selent J, Jacobs J, Rajagopal S. Phosphorylation barcode ensembles encoded by biased CXCR3 agonists direct non-redundant chemokine signaling. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.0R486. PM: 35554623.
Fordyce CB, Hill CL, Mark DB, Alhanti B, Pellikka PA, Hoffmann U, Patel MR, Douglas PS. Physician judgement in predicting obstructive coronary artery disease and adverse events in chest pain patients. Heart 2022 May 12;108(11):860-867. PM: 35110385.
Gardner J, Eiger D, Boldizsar N, Honeycutt CC, Kirchner S, Hicks C, Choi I, Zheng K, Warman A, Smith J, Zhang J, Rajagopal S. Location Bias Contributes to Functionally Selective Responses of Biased CXCR3 Agonists to Regulate Inflammation. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.0R865. PM: 35555971.
Harrington J, Tseliou E, Shah S, Shah KS. Paying Homage to the Power of Proteomics: Insights Into Obesity and Heart Failure From the HOMAGE Trial. J Card Fail 2022 May;28(5):787-788. PM: 35304349.
Hicks CN, Eiger D, Gardner J, Boldizsar N, Honeycutt C, Choi I, Rajagopal S. Location Bias of G Protein-Coupled Receptor Kinases Promotes Biased Signaling at CXCR3. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.R2182. PM: 35554028.
Kohlmann T, Lee C, Rajagopal S. Determining the Requirements for Gαi:β-arrestin Complex Formation at G Protein-Coupled Receptors. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.R5812. PM: 35554641.
Krychtiuk KA, Granger CB. In older persons at risk for dementia, a multidomain approach reduced stroke and transient ischemic attack. Ann Intern Med 2022 May;175(5):JC55. PM: 35500268.
Krychtiuk KA, Newby LK. Moderna COVID-19 vaccine was linked to myocarditis or myopericarditis at 28 d (4.2 events/100 000 persons). Ann Intern Med 2022 May;175(5):JC58. PM: 35500266.
Lala A, Lopes RD, Mentz RJ. International Collaborations in Heart Failure: JCF in Latin America. J Card Fail 2022 May;28(5):695-696. PM: 35559918.
Lee C, Kohlmann T, Xiong X, Rajagopal S. Regulation of Endothelial Cell function by Integration of Gαi and β-arrestin signaling at Atypical Chemokine Receptor 3. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.R6324. PM: 35554058.
Lewis GD, Docherty KF, Voors AA, Cohen-Solal A, Metra M, Whellan DJ, Ezekowitz JA, Ponikowski P, Böhm M, Teerlink JR, Heitner SB, Kupfer S, Malik FI, Meng L, Felker GM. Developments in Exercise Capacity Assessment in Heart Failure Clinical Trials and the Rationale for the Design of METEORIC-HF. Circ Heart Fail 2022 May;15(5):e008970. PM: 35236099.
Li A, Liu S, Huang R, Ahn S, Lefkowitz RJ. Loss of Biased Signaling Specificity of the Angiotensin II Type 1 Receptor in Overexpressed Systems. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.R2797. PM: 35555965.
Lowenstern A, Alexander KP, Pagidipati NJ, Hill CL, Pellikka PA, Cooper LS, Alhanti B, Hoffmann U, Mark DB, Douglas PS. Presenting Symptoms in Patients Undergoing Coronary Artery Disease Evaluation: Association With Noninvasive Test Results and Clinical Outcomes in the PROMISE Trial. Circ Cardiovasc Qual Outcomes 2022 May;15(5):e008298. PM: 35369715.
Minhas AMK, Ijaz SH, Jamal S, Dani SS, Khan MS, Greene SJ, Fudim M, Warraich HJ, Shapiro MD, Virani SS, Nasir K, Khan SU. Trends in Characteristics and Outcomes in Primary Heart Failure Hospitalizations Among Older Population in the United States, 2004 to 2018. Circ Heart Fail 2022 May;15(5):e008943. PM: 35078346.
Mullens W, Martens P, Testani JM, Tang WHW, Skouri H, Verbrugge FH, Fudim M, Iacoviello M, Franke J, Flammer AJ, Palazzuoli A, Barragan PM, Thum T, Marcos MC, Miró Ò, Rossignol P, Metra M, Lassus J, Orso F, Jankowska EA, Chioncel O, Milicic D, Hill L et al. Renal effects of guideline-directed medical therapies in heart failure: a consensus document from the Heart Failure Association of the European Society of Cardiology. Eur J Heart Fail 2022 Apr;24(4):603-619. PM: 35239201.
Patel JN, Abramov D, Fudim M, Okwuosa IS, Rabkin DG, Chung JS. The heart transplant allocation change attenuates but does not eliminate blood group O waitlist outcome disadvantage. Clin Transplant 2022 May;36(5):e14620. PM: 35213753.
Pham U, Chundi A, Rajagopal S. Distinct Spatial Conformations and Trafficking Patterns of β-arrestin Isoforms in AT1R Signaling. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.L7742. PM: 35559563.
Price MJ, Valderrábano M, Zimmerman S, Friedman DJ, Kar S, Curtis JP, Masoudi FA, Freeman JV. Periprocedural Pericardial Effusion Complicating Transcatheter Left Atrial Appendage Occlusion: A Report From the NCDR LAAO Registry. Circ Cardiovasc Interv 2022 May;15(5):e011718. PM: 35369701.
Razaghizad A, Oulousian E, Randhawa VK, Ferreira JP, Brophy JM, Greene SJ, Guida J, Felker GM, Fudim M, Tsoukas M, Peters TM, Mavrakanas TA, Giannetti N, Ezekowitz J, Sharma A. Clinical Prediction Models for Heart Failure Hospitalization in Type 2 Diabetes: A Systematic Review and Meta-Analysis. J Am Heart Assoc 2022 May 17;11(10):e024833. PM: 35574959.
Remillard TC, Cronley AC, Pilch NA, Dubay DA, Willner IR, Houston BA, Jackson GR, Inampudi C, Ramu B, Kilic A, Fudim M, Wright SP, Hajj ME, Tedford RJ. Hemodynamic and Clinical Determinants of Left Atrial Enlargement in Liver Transplant Candidates. Am J Cardiol 2022 Jun 1;172:121-129. PM: 35341576.
Van Belle E, Patel M, Davies J. Fractional Flow Reserve-Guided PCI as Compared with Coronary Bypass Surgery. N Engl J Med 2022 May 12;386(19):1863-1864. PM: 35544399.
Yaranov DM, Jefferies JL, Silver MA, Burkhoff D, Rao VN, Fudim M. Discordance of Pressure and Volume: Potential Implications for Pressure-Guided Remote Monitoring in Heart Failure. J Card Fail 2022 May;28(5):870-872. PM: 35158025.
Zeitouni M, Marquis-Gravel G, Smilowitz NR, Zakroysky P, Wojdyla DM, Amit AP, Rao SV, Wang TY. Prophylactic Mechanical Circulatory Support Use in Elective Percutaneous Coronary Intervention for Patients With Stable Coronary Artery Disease. Circ Cardiovasc Interv 2022 May;15(5):e011534. PM: 35580202.
Zhang Y, Kontos CD, Annex BH, Popel AS. Endothelial Regulation of Microvascular Growth and Stability by Ang-Tie and VEGF Signaling Pathways: A Mechanistic Computational Systems Biology Model. FASEB J 2022 May;36 Suppl 1:10.1096/fasebj.2022.36.S1.R2072. PM: 35560284.
Zhu H, Yin X, Holley CL, Meyer KD. Improved Methods for Deamination-Based mA Detection. Front Cell Dev Biol 2022 Apr 27;10:888279. PM: 35573664.
Duke Heart Pulse – week ending May 15th 2022
Highlights of the week:
Wang Receives Lifetime Achievement Award at QCOR22

Congratulations to Tracy Y. Wang, MD, professor of medicine in cardiology, director of Health Services & Outcomes Research, and Duke Clinical Research Institute member, has received the American Heart Association’s Council on Quality of Care and Outcomes Research (QCOR) 2022 Outstanding Lifetime Achievement Award! The award was presented earlier this weekend during the QCOR Scientific Sessions (May 13-14) in Reston, VA. Wang gave the keynote address.
The QCOR lifetime achievement award is presented to a QCOR council member for their significant long-term contributions to outcomes research and the improvement of cardiovascular care. Candidates are selected annually by QCOR’s nominating committee and the winner is selected by their leadership committee.
“Well, I guess this award makes me officially old now,” said Wang ahead of the award presentation. “Duke has such a unique environment that has allowed me to explore my interests and grow in delightfully unexpected ways. I’ve benefited from incredible mentorship, and am rejuvenated daily working alongside creative younger minds who want to make a difference in how we take care of patients.”
She received a number of accolades on Twitter, including:
“There’s no smarter researcher, more supportive mentor, or better human being in cardiology.” – Alex Fanaroff, MD, former Duke cardiology fellow.
“She is a brilliant physician scientist, and more importantly a truly wonderful person. Well deserved. Just wondering what she’ll do with the second half of her life???” — Women as One
“Exceptional clinician, researcher, educator, leader, sponsor, mentor, and friend.” — Vanessa Blumer, MD, Duke cardiology fellow.
“Such a well-deserved honor. Had to travel to Reston VA to see her IRL!”– Rob Mentz, MD
In addition to Wang, a number of current and former Duke faculty and fellows presented at QCOR including Emily O’Brien, Lesley Curtis, Alex Fanaroff, Mike Nanna, Jenn Rymer, Ajar Kochar, Rob Mentz, Vanessa Blumer, and Stephen Greene.
A perspective piece by Wang – “Mentorship and the Leaky Pipeline in Academic Cardiology” — was published in Circulation: Cardiovascular Quality and Outcomes during her award speech on Friday. A link to it can be found here: https://duke.is/yy65w.
Congratulations, Tracy! We are so proud of you – way to go!


Update: High-Sensitivity Troponin I (hsTnI), Effective 5/17 at DUH
Beginning May 17, 2022, High-Sensitivity Troponin I (hsTnI) will replace the current High-Sensitivity Troponin T test at Duke University Hospital. There will be no fundamental changes to the hsTn algorithm, results/interpretations reporting, or ordering. The hsTnI numerical thresholds are nearly identical to those for hsTnT, and the interpretations and disposition guidance that go with them will be available as currently and are unchanged.
Additional information is available through the following links:
High Sensitivity Troponin I for Providers: https://intranet.dh.duke.edu/sites/MaestroCare/Maestro%20Care%20Training%20Supplements/High%20Sensitivity%20Troponin%20I%20for%20Providers.pdf
Troponin I Smarttext tipsheet (PPT): https://intranet.dh.duke.edu/sites/MaestroCare/Maestro%20Care%20Training%20Supplements/Troponin%20I%20Smarttext%20tipsheet.pptx?d=wb2ba5706a7da4939bd620ddc971b5d21
SOM Faculty Awards Dinner Honors 2020-2022 Awardees
The Duke School of Medicine annual faculty awards dinner was held this week at the Sarah Duke Gardens. A number of Duke Heart faculty members were in attendance, including Cary Ward, Carmelo Milano and Manesh Patel – our 2022 awardees. Due to the pandemic, the awards dinner had not been held in person for two years. Awardees for 2020 or 2021 were invited to join the festivities. A recap of our current and past awardees:


- Ward and Milano were co-winners of the 2022 Palumbo award which recognizes dedication to compassionate patient care and excellence in the teaching and mentoring of young physicians.
- Manesh Patel received the 2022 Career Mentoring Award in Clinical Research/Population Health.
- 2021: Kevin Thomas was the recipient of the Excellence in Professionalism Award, which recognizes the importance of promoting ethical and professional behavior in our community.
- 2021: Robert Mentz received the Early Career Research Mentoring Award in Clinical/Population Health Science.
- 2021: Terry Fortin received the Master Clinician/Teacher Award, which honors individuals with superlative accomplishment and service in the areas of clinical care and teaching
- 2020: Larry Crawford received the Excellence in Professionalism Award. As noted above, the award is given to a faculty member that exemplifies ethical and professional behavior in our community. Recipients represent Duke’s guiding principles of respect, trustworthiness, diversity, teamwork, and learning.
- 2020: Mike Sketch received the Leonard Tow Humanism in Medicine Award.
- 2020: Tracy Wang received the Early Career Mentoring Award in Clinical/Population Health Science.
We are so proud of each one of you. Congratulations!





2022 AATS Underway in Boston
The American Association for Thoracic Surgery’s 102nd annual meeting is underway in Boston (May 14-17) and we’re giving a shout-out to all Duke team members in attendance!

A very special congratulations to Jeff Gaca, MD and Jacob Klapper, MD – both surgeons were elected to AATS and officially inducted this weekend. Such great news! Founded in 1917, the American Association for Thoracic Surgery (AATS), is comprised of more than 1,500 of the world’s foremost cardiothoracic surgeons from 46 countries. We are excited for both of them.
We’ll have coverage of key Duke presentations next weekend.

Arlene Martin Departs Fellowship Program
We are saddened to have said goodbye to one of our long-term Duke Heart team members this week. Arlene Martin, our wonderful GME program coordinator for the Cardiovascular Disease fellowship, the Advanced Training in Cardiology fellowship, and the Clinical Investigator Pathway-Cardiovascular Disease fellowship has left Duke in order to focus on family needs. Her last day with us was May 11.
Arlene has worked closely with the fellowship program for more than a decade — and it’s hard to imagine the fellowship program without her. She has done an incredible job for us and for our fellows!
From Anna Lisa Chamis, MD, current program director:
“Arlene has diligently served as program coordinator for multiple Division of Cardiology fellowships since 2011. During that time, she supported 9 program directors and ~140 trainees. Notably, she helped launch 2 new ACGME fellowship programs at Duke and spearheaded the initial site accreditation for those programs. Arlene also worked tirelessly to help us apply for grants/ external funding to support our fellowship programs, assisting in the acquisition of $2.3 million in salary and benefits for our fellowship programs during her tenure. Not surprisingly, she was awarded the 2015-2016 Fellows’ staff service award. Personally, Arlene has taught me so much about the administrative regulations and policies surrounding our programs, and I am grateful to have benefitted from her vast knowledge and experience.”
From Andrew Wang, MD:
“Arlene actually began her work at Duke as my administrative assistant, but helped with tasks for the previous program coordinator too. When the program coordinator role became available, she expressed her interest, applied, and was clearly the most qualified candidate (even with little knowledge of ACGME requirements at that time). In nearly 10 years of working with her as our program coordinator, she was dedicated to improving our program as well as the experience and environment for our fellows. She made important and lasting improvements in our fellowship program. She brought our program from the “paper chart” era to the electronic era. She took on new responsibilities and learned new skills, including grant-writing to support our fellows, with rapid adeptness and competency. In all of her work, she demonstrates a strong sense of ownership, conscientiousness, timeliness, and high quality. I wish her the best in her future endeavors and thank her for her support and contributions to our fellowship program.”
From Svati Shah, MD:
“Arlene has done an incredible job as the Cardiology Fellowship Program Director! I had the honor of being an Associate Program Director with Arlene for many years. She has balanced the intense responsibilities of this job beautifully. She did so much work quietly behind the scenes to make sure we had a robust (and compliant!) fellowship. I am so grateful for how much she taught me and helped me grow as an APD. She will be greatly missed.”
From Amanda Coniglio, MD, (outgoing chief cardiology fellow)
“Arlene has always gone above and beyond to make sure the fellows and program were supported. She has paid meticulous attention to detail and has always been quick to help when needed. She will be greatly missed!”
From Christopher Wrobel, MD (incoming chief cardiology fellow):
“Arlene has been an invaluable asset to the fellowship. She has superhuman organizational prowess that I hope to have a fraction of some day. She has always been understanding of my (occasional) lapses, and gently guided me on the road to full compliance. I know I and all of the other fellows will remain greatly indebted to Arlene for all of her work over the years. We will miss you greatly Arlene!”
She truly has been a behind-the-scenes person helping make “all the things” happen. Thank you so much for all you’ve done for us, Arlene! We wish you all the best!
ICYMI: Frazier-Mills Interviewed by HeartRhythm TV
Camille Frazier-Mills, MD appears in a recent episode of the Women in EP – Mentorship Series on HeartRhythm TV (YouTube). The topic last weekend was Heart Rhythm Society DEI Council: Inclusion Series, Closing the Sex Gap. She was interviewed along with Annabelle Volgman of Rush University Medical Center. Among other factors, Frazier Mills says early exposure and mentorship are key to getting more women to specialize in electrophysiology. This is definitely worth watching! Check it out here: https://duke.is/ru8mb.
D’Amico Named Associate Editor, Annals of Surgery
 Congratulations to Thomas D’Amico, MD, the Gary Hock Endowed Professor of Surgery and Chief, Section of General Thoracic Surgery in the Division of Cardiovascular and Thoracic Surgery. He was recently named associate editor for thoracic surgery for the journal Annals of Surgery. D’Amico is currently serving a two-year term as medical director of the AATS.
Congratulations to Thomas D’Amico, MD, the Gary Hock Endowed Professor of Surgery and Chief, Section of General Thoracic Surgery in the Division of Cardiovascular and Thoracic Surgery. He was recently named associate editor for thoracic surgery for the journal Annals of Surgery. D’Amico is currently serving a two-year term as medical director of the AATS.
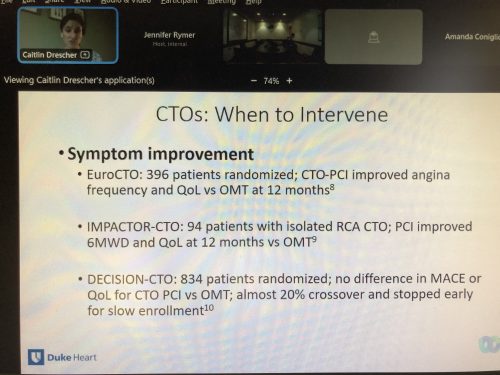
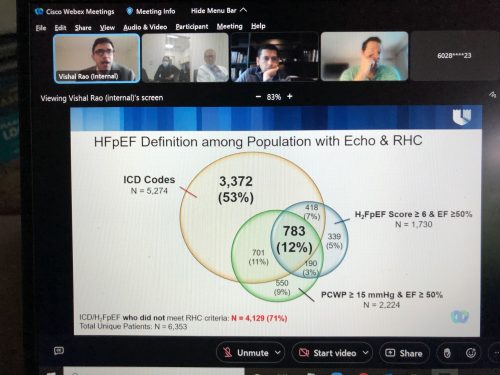
Dresher & Rao Presented CGR
We had two terrific cardiology grand rounds presentations this past week. On Tuesday, cardiology fellow Caitlin Dresher presented on coronary CTOs and cardiac MRI, and on Thursday, cardiology fellow Vishal Rao presented on gaps in care delivery and phenotyping across the spectrum of heart failure along with strategies for improvement. Nicely done!
Nurses Week 2022: Our 1st Daisy Award!
We want to close out Nurses Week with another round of thanks to all our terrific Duke Heart nurses! We hope you enjoyed some of the special events that were held to celebrate you this past week. Shown here are Duke Heart CVSSU RNs enjoying mid-morning Coffee Cart with Mary Lindsay and Joe Kelly!


In other great news this week, we learned that Zac Snell, RN on 6East has received the first DAISY Award for the Heart Center! The awards are given by the Daisy Foundation, which is an international foundation that was formed in November 1999 by the family of J. Patrick Barnes, a patient who passed away due to complications of Idiopathic Thrombocytopenic Purpura (ITP). The nursing care that Patrick received when hospitalized profoundly touched his family; they launched the Foundation in his memory. Nurses who demonstrate extraordinary and compassionate care are nominated by patients and family members.
Zac is pictured below with 6E team members, Heart Center leadership, and leadership from DUH. Great job, Zac! Well done.
The week culminated with the annual Friends of Nursing Gala, which was held last night. We will have coverage of all Duke Heart winners and photos next weekend!

COVID-19 Update
All the latest Clinical Operations updates related to COVID can be found at https://covid-19.dukehealth.org. Patient-facing resources on DukeHealth.org can be found here: https://www.dukehealth.org/covid-19-update/resources. Duke University maintains a resource page as well, which can be accessed here: https://coronavirus.duke.edu/updates/for-staff.
Upcoming Events & Opportunities
Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged. Submissions by Noon, Wednesdays, to be considered for weekend inclusion.
Duke Heart in the News:
May 10 — Duke Hospital, Duke Regional, Duke Raleigh
Newsobserver.com
NC claims top spot for nation’s safest hospitals. See how Triangle hospitals rank
https://duke.is/n7dts
May 10 — Richard Shannon and Beverly Gray
CBS17.com
Duke Health doctors worry about abortion ban impacts
https://duke.is/5pv96
May 12 — Michelle Kelsey
CBS17.com/WNCN
How you brew coffee could impact your cholesterol, research shows
https://duke.is/bjdvy
Division of Cardiology Publications Indexed in PubMed April 28 – May 11, 2022
Ahmed F, Abid M, Maniya T, Usman MS, Fudim M.Incidence and prognosis of COVID-19 amongst heart transplant recipients: a systematic review and meta-analysis. Eur J Prev Cardiol 2022;29(6):e224-e226. PM: 34757386.
Alenezi F, Covington TA, Mukherjee M, Mathai SC, Yu PB, Rajagopal S. Novel Approaches to Imaging the Pulmonary Vasculature and Right Heart. Circ Res 2022;130(9):1445-1465. PM: 35482838.
Anand SS, Hiatt W, Dyal L, Bauersachs R, Berkowitz SD, Branch KRH, Debus S, Fox KAA, Liang Y, Muehlhofer E, Nehler M, Haskell LP, Patel M, Szarek M, Yusuf S, Eikelboom J, Bonaca MP. Low-dose rivaroxaban and aspirin among patients with peripheral artery disease: a meta-analysis of the COMPASS and VOYAGER trials. Eur J Prev Cardiol 2022;29(5):e181-e189. PM: 34463737.
Andonian BJ, Koss A, Koves TR, Hauser ER, Hubal MJ, Pober DM, Lord JM, MacIver NJ, St Clair EW, Muoio DM, Kraus WE, Bartlett DB, Huffman KM. Rheumatoid arthritis T cell and muscle oxidative metabolism associate with exercise-induced changes in cardiorespiratory fitness. Sci Rep 2022;12(1):7450. PM: 35523821.
Assimon MM, Pun PH, Al-Khatib SM, Brookhart MA, Gaynes BN, Winkelmayer WC, Flythe JE. Proton pump inhibitors may enhance the risk of citalopram- and escitalopram-associated sudden cardiac death among patients receiving hemodialysis. Pharmacoepidemiol Drug Saf 2022;31(6):670-679. PM: 35285107.
Bachour K, Dodge SE, Kearing S, Douglas PS, Wong S, Coylewright M. Predicting When Women Will Achieve Equitable Representation in Four Specialties: The WHEN Study. Am J Med 2022;135(5):650-653. PM: 35134367.
Baggish AL, Chang CJ, Drezner JA, Harmon KG, Kraus WE, Matuszak J, Wasfy MM. ACSM-AMSSM Call to Action: Adapting Preparticipation Cardiovascular Screening to the COVID-19 Pandemic. Curr Sports Med Rep 2022;21(5):159-162. PM: 35522440.
Bernstein E, Wang TY. Point-of-Care Ultrasonography: Clearly More Than a Pretty Picture-Reply. JAMA Intern Med 2022;182(5):568. PM: 35285852.
Blankstein R, Shaw LJ, Gulati M, Atalay MK, Bax J, Calnon DA, Dyke CK, Ferencik M, Heitner JF, Henry TD, Hung J, Knuuti J, Lindner JR, Phillips LM, Raman SV, Rao SV, Rybicki FJ, Saraste A, Stainback RF, Thompson RC, Williamson E, Nieman K, Tremmel JA, et al. Implications of the 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/SCMR Chest Pain Guideline for Cardiovascular Imaging: A Multisociety Viewpoint. JACC Cardiovasc Imaging 2022;15(5):912-926. PM: 35512960.
De Caterina R, Patti G, Westerbergh J, Horowitz J, Ezekowitz JA, Lewis BS, Lopes RD, McMurray JJV, Atar D, Bahit MC, Keltai M, López-Sendón JL, Ruzyllo W, Granger CB, Alexander JH, Wallentin L. Heterogeneity of diabetes as a risk factor for major adverse cardiovascular events in anticoagulated patients with atrial fibrillation: an analysis of the ARISTOTLE trial. Eur Heart J Cardiovasc Pharmacother 2022;8(3):227-235. PM: 33367487.
Frankel DS, Dechert-Crooks BE, Campbell K, DeSimone CV, Etheridge S, Harvey M, Lampert R, Nayak HM, Saliba WI, Shea J, Thomas J, Zado E, Daubert JP. 2021 HRS Educational Framework for Clinical Cardiac Electrophysiology. Heart Rhythm O2 2022 Apr 15;3(2):120-132. PM: 35496459.
Freeman JV, Higgins AY, Wang Y, Du C, Friedman DJ, Daimee UA, Minges KE, Pereira L, Goldsweig AM, Price MJ, Reddy VY, Gibson D, Doshi SK, Varosy PD, Masoudi FA, Curtis JP. Antithrombotic Therapy After Left Atrial Appendage Occlusion in Patients With Atrial Fibrillation. J Am Coll Cardiol 2022;79(18):1785-1798. PM: 35512858.
Friedman DJ, Du C, Wang Y, Agarwal V, Varosy PD, Masoudi FA, Holmes DR, Reddy VY, Price MJ, Curtis JP, Freeman JV. Patient-Level Analysis of Watchman Left Atrial Appendage Occlusion in Practice Versus Clinical Trials. JACC Cardiovasc Interv 2022;15(9):950-961. PM: 35512918.
Fudim M, Kaye DM, Borlaug BA, Shah SJ, Rich S, Kapur NK, Costanzo MR, Brener MI, Sunagawa K, Burkhoff D. Venous Tone and Stressed Blood Volume in Heart Failure: JACC Review Topic of the Week. J Am Coll Cardiol 2022;79(18):1858-1869. PM: 35512865.
Goldberg LR, Jorbenadze A, Shaburishvilli T, Mirro MJ, Fudim M, Zuber M, Stämpfli SF, Tanner FC, Erne P, Cleland JG. Synchronized diaphragmatic stimulation: a case report of a novel extra-cardiac intervention for chronic heart failure. ESC Heart Fail 2022;9(3):1677-1681. PM: 35297198.
Harskamp RE, Lucassen WAM, Lopes RD, Himmelreich JCL, Parati G, Weert HCPMV. Risk of stroke and bleeding in relation to hypertension in anticoagulated patients with atrial fibrillation: a meta-analysis of randomised controlled trials. Acta Cardiol 2022;77(3):191-195. PM: 33685380.
Jain V, Minhas AMK, Khan SU, Greene SJ, Pandey A, Van Spall HGC, Fonarow GC, Mentz RJ, Butler J, Khan MS. Trends in HF Hospitalizations Among Young Adults in the United States From 2004 to 2018. JACC Heart Fail 2022;10(5):350-362. PM: 35483798.
Jimenez Contreras F, Mendiola Pla M, Schroder J, Bryner B, Agarwal R, Russell SD, Mirza J, Daneshmand MA, Milano C. Progression of aortic valve insufficiency during centrifugal versus axial flow left ventricular assist device support. Eur J Cardiothorac Surg 2022;61(5):1188-1196. PM: 35167677.
Kelsey MD, Nelson AJ, Green JB, Granger CB, Peterson ED, McGuire DK, Pagidipati NJ. Guidelines for Cardiovascular Risk Reduction in Patients With Type 2 Diabetes: JACC Guideline Comparison. J Am Coll Cardiol 2022;79(18):1849-1857. PM: 35512864.
Malenka DJ, Bhatt DL, Bradley SM, Shahian DM, Draoui J, Segawa CA, Koutras C, Abbott JD, Blankenship JC, Vincent R, Windle J, Tsai TT, Curtis J, Roe M, Masoudi FA. The National Cardiovascular Data Registry Data Quality Program 2020: JACC State-of-the-Art Review. J Am Coll Cardiol 2022;79(17):1704-1712. PM: 35483759.
Manichaikul A, Lin H, Kang C, Yang C, Rich SS, Taylor KD, Guo X, Rotter JI, Craig Johnson W, Cornell E, Tracy RP, Peter Durda J, Liu Y, Vasan RS, Adrienne Cupples L, Gerszten RE, Clish CB, Jain D, Conomos MP, Blackwell T, Papanicolaou GJ, Rodriguez A. Lymphocyte activation gene-3-associated protein networks are associated with HDL-cholesterol and mortality in the Trans-omics for Precision Medicine program. Commun Biol 2022;5(1):362. PM: 35501457.
Muiruri C, Corneli A, Cooper L, Dombeck C, Gray S, Longenecker CT, Meissner EG, Okeke NL, Pettit AC, Swezey T, Vicini J, Bloomfield GS. Perspectives of HIV specialists and cardiologists on the specialty referral process for people living with HIV: a qualitative descriptive study. BMC Health Serv Res 2022;22(1):623. PM: 35534889.
Narcisse DI, Katzenberger DR, Gutierrez JA. Contemporary Medical Therapies for Patients with Peripheral Artery Disease and Concomitant Type 2 Diabetes Mellitus: a Review of Current Evidence. Curr Cardiol Rep 2022;24(5):567-576. PM: 35201560.
Nelson AJ, Haynes K, Shambhu S, Eapen Z, Cziraky MJ, Nanna MG, Calvert SB, Gallagher K, Pagidipati NJ, Granger CB . High-Intensity Statin Use Among Patients With Atherosclerosis in the U.S. J Am Coll Cardiol 2022;79(18):1802-1813. PM: 35512860.
Piccini JP, Arps K. Sacubitril/Valsartan Therapy for AF and HFpEF: Is the Glass Half Empty or Half Full? JACC Heart Fail 2022;10(5):347-349. PM: 35483797.
Roselli C, Yu M, Nauffal V, Georges A, Yang Q, Love K, Weng LC, Delling FN, Maurya SR, Schrölkamp M, Tfelt-Hansen J, Hagège A, Jeunemaitre X, Debette S, Amouyel P, Guan W, Muehlschlegel JD, Body SC, Shah S, Samad Z, Kyryachenko S, Haynes C, Rienstra M, et al. Genome-wide association study reveals novel genetic loci: a new polygenic risk score for mitral valve prolapse. Eur Heart J 2022;43(17):1668-1680. PM: 35245370.
Rymer JA, Gutierrez JA. Challenges in Peripheral Artery Disease Clinical Trial Implementation and Design. Can J Cardiol 2022;38(5):699-702. PM: 35074414.
Salah HM, Levin AP, Fudim M. Updates from the American Heart Association Scientific Sessions: cardiovascular pharmacotherapy. Eur Heart J Cardiovasc Pharmacother 2022;8(3):E4-E6. PM: 34864960.
Selvaraj S, Margulies KB, Dugyala S, Schubert E, Tierney A, Arany Z, Pryma DA, Shah SH, Rame JE, Kelly DP, Bravo PE. Comparison of Exogenous Ketone Administration Versus Dietary Carbohydrate Restriction on Myocardial Glucose Suppression: A Crossover Clinical Trial. J Nucl Med 2022;63(5):770-776. PM: 34675108.
Sidhu MS, Alexander KP, Huang Z, O’Brien SM, Chaitman BR, Stone GW, Newman JD, Boden WE, Maggioni AP, Steg PG, Ferguson TB, Demkow M, Peteiro J, Wander GS, Phaneuf DC, De Belder MA, Doerr R, Alexanderson-Rosas E, Polanczyk CA, Henriksen PA, Conway DSG, et al. Causes of cardiovascular and noncardiovascular death in the ISCHEMIA trial. Am Heart J 2022;248:72-83. PM: 35149037.
Smith PJ, Sherwood A, Hinderliter AL, Mabe S, Tyson C, Avorgbedor F, Watkins LL, Lin PH, Kraus WE, Blumenthal JA. Cerebrovascular Function, Vascular Risk, and Lifestyle Patterns in Resistant Hypertension. J Alzheimers Dis 2022;87(1):345-357. PM: 35275539.
Spertus JA, Mack MJ, Ohman EM. Improving the National Cardiovascular Data Registry’s Value to Elevate the Quality of Cardiovascular Care. J Am Coll Cardiol 2022;79(17):1713-1716. PM: 35483760.
Spitzer E, Fanaroff AC, Gibson CM, Seltzer J, McFadden E, Ali M, Wilson M, Menon V, Mehran R, Held C, Mahaffey KW, Lopes RD. Independence of clinical events committees: A consensus statement from clinical research organizations. Am Heart J 2022;248:120-129. PM: 35296411.
Tanaka A, Hebert AM, Smith-Washington A, Hoffstaetter T, Goldenberg R, Vemulapalli S, Del Río-Solá L, Arnaoutakis GJ, Mussa F, Ota T. Knowledge gaps in surgical management for aortic dissection. Semin Vasc Surg 2022;35(1):35-42. PM: 35501039.
Verma S, Rathwell S, Fremes S, Zheng Y, Mehta R, Lopes RD, Alexander JH, Goodman SG, Diepen SV. Associated factors and clinical outcomes in mechanical circulatory support use in patients undergoing high risk on-pump cardiac surgery: Insights from the LEVO-CTS trial. Am Heart J 2022;248:35-41. PM: 35263653.
Wang A, Fosbøl EL. Current recommendations and uncertainties for surgical treatment of infective endocarditis: a comparison of American and European cardiovascular guidelines. Eur Heart J 2022;43(17):1617-1625. PM: 35029274.
Wegermann ZK, Mack MJ, Arnold SV, Thompson CA, Ryan M, Gunnarsson C, Strong S, Cohen DJ, Alexander KP, Brennan JM. Anxiety and Depression Following Aortic Valve Replacement. J Am Heart Assoc 2022;11(9):e024377. PM: 35470691.
Wilson BS, Tucci DL, Moses DA, Chang EF, Young NM, Zeng FG, Lesica NA, Bur AM, Kavookjian H, Mussatto C, Penn J, Goodwin S, Kraft S, Wang G, Cohen JM, Ginsburg GS, Dawson G, Francis HW. Harnessing the Power of Artificial Intelligence in Otolaryngology and the Communication Sciences. J Assoc Res Otolaryngol 2022;23(3):319-349. PM: 35441936.
Duke Heart Pulse – Week Ending May 8th 2022 – Mother’s Day
Chief’s message:
Mother’s Day and appreciating the Moms in our Lives!
Mother’s Day around Duke and UNC is also noted for college, medical school, and post-graduate degree graduations. It is a good tradition allowing family’s to relish an important milestone and provide the opportunity to consider the influence mothers have on our lives.We hope that you all got to spend some time with the ones you love appreciate all the moms out in the Duke Heart community and the lessons of love, kindness, and selfless devotion they have on us all. Mothers come in many iterations – to those we are blessed to have among us, and those who have passed before us — we hope this has been a wonderful weekend for all!
Highlights of the Week.
Harrington gives Medicine Grand Rounds as Joseph C. Greenfield Visiting Professor
We welcomed Robert Harrington, chair of the Department of Medicine at Stanford, back to campus this week as the Joseph C. Greenfield Visiting Professor. His lecture, Cardiovascular Medicine as a Data Science was presented during Medicine Grand Rounds on Friday. It was great to see so many residents, faculty and fellows that could attend. Bob Harrington was able to provide an amazing over-arching view of not only how medicine has become a data science field, but more importantly providing many examples of how clinicians and data scientists are interacting to do clinical research, engage patients, and deliver care. It was a fun to have Bob revisit the cath lab, the clinical wards, work with our residents and fellows to discuss how we can continue to improve medicine. The innovation on getting data science and information at the point of care at Stanford Medicine was quite impressive.

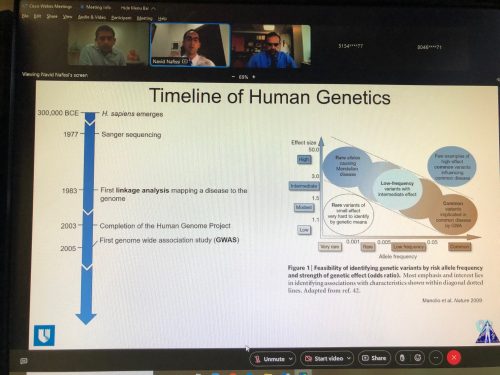
Nafissi Grand Rounds Presentations
Navid Nafissi gave an excellent presentation this week during Cardiology Grand Rounds on Tuesday evening. His topic was “Precision Medicine in Arrhythmias: Not Your Daddy’s Long QT”. In keeping with the data science theme – Navid highlighted how our understanding of arrhythmias and the genetic and clinical correlates is exploding requiring a broad set of skills for clinicians in this area.
Nurses Week 2022
It’s Nurses Week, 2022 (May 6-12)! On behalf of Duke Heart, we would like to recognize each of our nurses for their professiona l accomplishments and contributions in caring for Duke Heart patients over the past year. This year continues to be challenging with the ongoing COVID pandemic and more patients than ever in need of the highly specialized care that only the Duke Heart team can provide.
l accomplishments and contributions in caring for Duke Heart patients over the past year. This year continues to be challenging with the ongoing COVID pandemic and more patients than ever in need of the highly specialized care that only the Duke Heart team can provide.
Duke Heart Nurses are foundational to Duke’s ability to provide best-in-class heart care. Each of our nurses have been a part of many firsts in the U.S. and at Duke. These firsts include caring for patients and partnering with our cardiology and cardiac surgery providers in landmark clinical trials including the TransMedics DCD trials and the implant of the first-in-U.S. Carmat total artificial heart last summer. At Duke University Hospital, Duke Heart Nurses supported bed and tower expansion, growth of CICU and cardiology beds and grew the emergency response teams including the addition of a Behavioral Response team. Our outpatient teams continued to support our patients and families using new technologies and approaches, including enhanced telehealth and mobile cardiac rehabilitation. None of these accomplishments would be possible without the amazing care across our outpatient, rehabilitation, procedural, and diagnostic teams and the inpatient cardiology and surgical units.
In the midst of a busy clinical year, each of them continued to show tremendous compassion for not only Duke patients and families but also each other and our community. The Duke Heart Nursing team possesses unmatched talent, dedication and teamwork that exemplifies living the Duke Values.
Kudos and Thank you!
Celebrating Perfusionists!
 Our Duke Perfusion team, one of the largest in the country, has a scope of practice inclusive of cardiopulmonary bypass, extracorporeal support, mechanical circulatory support, and autotransfusion for adult and pediatric patients. Areas of expertise include major aortic surgery, advanced heart failure, heart and lung transplantation, minimally invasive and robotic surgery, blood conservation, surgical oncology, and complex congenital surgery. Our team has been involved in multiple groundbreaking innovations including Transmedics OCS heart procurements, cutting-edge mechanical support and laboratory research. Duke perfusionists are nationally recognized leaders in the field and serve as clinical instructors for four perfusion schools.
Our Duke Perfusion team, one of the largest in the country, has a scope of practice inclusive of cardiopulmonary bypass, extracorporeal support, mechanical circulatory support, and autotransfusion for adult and pediatric patients. Areas of expertise include major aortic surgery, advanced heart failure, heart and lung transplantation, minimally invasive and robotic surgery, blood conservation, surgical oncology, and complex congenital surgery. Our team has been involved in multiple groundbreaking innovations including Transmedics OCS heart procurements, cutting-edge mechanical support and laboratory research. Duke perfusionists are nationally recognized leaders in the field and serve as clinical instructors for four perfusion schools.
The Duke Perfusion team is devoted to our community and engages in multiple outreach and service initiatives each year. To celebrate Perfusion Week (May 1-7), the team volunteered with Habitat Build.
An outstanding group in any year, this team has put in an incredible effort during the pandemic and we are extremely proud of them. Great job!!!

Kudos to Hughes & Burkett
 We received the following note this week via Press Ganey in regard to care provided to a patient by
We received the following note this week via Press Ganey in regard to care provided to a patient by

Chad Hughes and Melissa Burkett:
“I would like to comment on Dr. Hughes first, then his assistant Melissa. I doubt anything I say hasn’t been said before about Dr. Hughes or Melissa, but perhaps substantiates comments made by others. I found both of these professionals to be world class. Dr. Hughes reminds me of a military special operator or fighter pilot I have met and worked with in my career. I know the personality well. Dr. Hughes is laser focused, precise, and highly motivated. He’s EXACTLY what you would want in a surgeon. The bonus is he puts you at ease immediately. Perhaps it’s his demeanor or level of confidence, but make no mistake you know when talking with him he knows his craft very well. He’s obviously highly trained and skilled. I would venture to guess if medicine had not called him, he would have been a Green Beret, Navy SEAL, or fighter pilot. And if you were going into an operation, you would want him on your TEAM. He’s on point, and will get the job done better than probably 99.9% of surgeons in the world (that’s my after-action report). Generally, you cannot help but like the guy. And his assistant, Melissa, who must work a crazy schedule, always manages to follow up with every question or concern you may have. I am not sure what anyone would expect or want in a medical care TEAM. Perhaps Dr. Hughes and Melissa are the special forces of Duke Medical.” — A grateful patient, name withheld for confidentiality
“THANK YOU for the great things you are doing for our patients every day!” — Jamie Hilton, Nurse Manager, Operations
Well done, Chad & Melissa!

ACC Leadership Academy Held
The ACC Emerging Faculty Leadership Academy was held May 1-3 at Heart House in Washington, DC. Four invited participants had ties to Duke Heart. Here they are together, shown L-R are: Tony Gutierrez, Lauren Cooper, cardiology fellow from 2012-2016; Kristen Campbell, clinical pharmacist with Duke EP, and Kelly Schlendorf, advanced heart failure fellow, 2011 – 2012. Congrats to all of you and a hat tip to Kristen Campbell for the photo!

Tannu Recognized by ASE Foundation
 We are pleased to share that Manasi Tannu, a first-year cardiology fellow, has been recognized by the ASE Foundation with a Top Investigator Travel Grant.
We are pleased to share that Manasi Tannu, a first-year cardiology fellow, has been recognized by the ASE Foundation with a Top Investigator Travel Grant.
We received a message from Fawaz Alenezi this week that read, “Our Duke echo lab abstracts that are led by our phenomenal fellow Manasi Tannu have been recognized as the ASE Foundation Top Investigators and will receive $1000 to support travel to attend the ASE meeting. The selected abstracts are:
- Echocardiography based estimation of pulmonary vascular resistance and outcomes in patients with pulmonary hypertension.
- Prognostic value of right ventricular-pulmonary artery coupling in patients with pulmonary hypertension.
The ASE Foundation is the philanthropic arm of the American Society of Echocardiography. Each year, the ASE Foundation works with the ASE Scientific Sessions Abstract Chairs to identify meritorious early career abstract presenters. The selected presenters are recognized as the ASE Foundation Top Investigators and each receives a travel grant in the amount of $1,000 (U.S. currency) to support their travel to attend the ASE meeting and present their accepted abstract(s).
In the announcement letter to Tannu, Andrea M. Van Hoever, Deputy Director of the ASE Foundation wrote, “Young investigators such as yourself are the scientific heart and future of ASE’s annual meeting. We are honored to be able to support your attendance and look forward to seeing you in Seattle.”
Way to go, Manasi!
COVID-19 Update
All the latest Clinical Operations updates related to COVID can be found at https://covid-19.dukehealth.org. Patient-facing resources on DukeHealth.org can be found here: https://www.dukehealth.org/covid-19-update/resources. Duke University maintains a resource page as well, which can be accessed here: https://coronavirus.duke.edu/updates/for-staff.
Upcoming Events & Opportunities
Cardiology Grand Rounds
May 10: Coronary CTOs and Cardiac MRI: The Duke Experience with Caitlin Dresher. 5 p.m., Webex.
May 12: Mind the Gaps: Novel Strategies for Care Delivery and Phenotyping Across the Spectrum of Heart Failure with Vishal Rao. 5 p.m., Webex link coming soon.
Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged. Submissions by Noon, Wednesdays, to be considered for weekend inclusion.
Duke Heart in the News:
April 28 — Manesh Patel
Healio/Cardiology
Asundexian confers lower bleeding rates vs. apixaban for stroke prevention in AF
https://duke.is/wjqbn
April 29 — Manesh Patel
HCP Live
Overview of Polyvascular Disease and Coronary Artery Disease
https://duke.is/pu7nq
April 29 — Jonathan Piccini
Cardiac Rhythm News
New data from STROKE AF trial shared at HRS 2022
https://duke.is/r8t5u
May 1 — Jonathan Piccini
Cardiovascular Business
STROKE AF study shows insertable cardiac monitors detect 4 times more AFib than Holter monitoring
https://duke.is/6tmma
May 1 — James Daubert
MedpageToday
Menstrual Cycles Point to Link Between Sex Hormones and Long QT
https://duke.is/5yp7j
May 1 — Joseph Turek
WCBS-NY (Radio)
Breakthrough could mean end of anti-rejection drugs for transplant patients
https://duke.is/nhtkd
May 2 — Sana Al-Khatib
Medscape
Apple Watch ECG App, Still Experimental, Reveals Asymptomatic Low LVEF
https://duke.is/cnyvt
May 3 — Daniel Friedman
tctMD
NCDR Analyses Offer Insights Into First-Generation Watchman Outcomes
https://duke.is/yqt4m
May 5 — Sana Al-Khatib
Healio
Apple Watch app, using AI, identifies left ventricular dysfunction
https://duke.is/pfkp6
May 5 — Sana Al-Khatib
Medscape (en español)
https://duke.is/rg6xf
Duke Heart Pulse – week ending May 1st 2022
Chief’s message:
Hope everyone had a good week and some time for rest. This was a busy week for Duke Heart with the Heart Rhythm Society (HRS) national meeting with several faculty and fellow presentations, the International Society for Heart & Lung Transplantation (ISHLT) 42nd Annual Meeting and Scientific Sessions in Boston with several important presentations from our Duke Heart Faculty and fellows including several clinical practice changing studies, the first in-person Heart Center Leadership Council meeting to review our progress in three years, and the Duke ACTIV-3 clinical research team, led by our own Peter K. Smith, MD — the team was presented with a Duke University Presidential Award. This all happened while we kept working hard to provide our patients the best opportunity for heart care – something that was again evident this weekend on the wards and in the cath lab. Our Heart Center Leadership council Chair – Bob Keegan wanted to make sure that on behalf of the Heart Center Leadership council we include a tremendous thanks to all employees across Duke Heart on their behalf of the council in this weekend’s issue of Pulse. Appreciate the support Bob!
Hopefully as we approach the end of the academic year we will have an opportunity to celebrate our fellows, faculty and staff at some of our end of year events.
Highlights of the week:
ACTIV-3, Global Efforts, Transplant Nurses & Perfusion Week
We have so much to celebrate! First, happy May Day, traditionally the halfway point between the spring equinox and the summer solstice, according to the Farmer’s Almanac. With spring well underway here in NC, today also kicks off Perfusion Week 2022, May 1-7, so be sure to thank our amazing perfusionists when you see them!
Several cardiologists and their global efforts were featured in a new Magnify article out this week; our ACTIV-3 team received the prized Duke University Presidential Award (see below), we wrapped up Patient Experience Week (April 25-29), National Donate Life month (April) and Transplant Nurses Week runs through tomorrow, May 2. Duke is blessed with one of the best transplant teams in the world, and our nurses are a big part of that! We especially thank the nurses supporting our lung and heart transplant surgical teams and all those caring for our transplant patients pre- and post-surgery. We could not do this without you!
Speaking of transplant teams…
Duke Heart Shines at ISHLT 2022
The International Society for Heart & Lung Transplantation (ISHLT) 42nd Annual Meeting and Scientific Sessions were held April 27-30 in Boston.
ICYMI, the U.S. Food and Drug Administration this week granted premarket approval to TransMedics for its OCS Heart System for use with organs from donors after circulatory death (DCD). The TransMedics OCS Heart System is now approved with the extended clinical indication for ex vivo reanimation, functional monitoring, and beating-heart preservation of DCD hearts. This indication is based on the results of the OCS DCD Heart Trial and the associated Continued Access Protocol (EXPAND trial) which were presented by Jacob Schroder, MD, on Friday, April 29 at ISHLT.

“The FDA’s approval of the OCS for DCD donor hearts is the natural progression from the prior approval of the device for extended criteria brain dead donors, supported by the excellent results from the U.S. DCD trial,” said Schroder, surgical director of heart transplantation at Duke University Health System and the principal investigator for the OCS DCD Heart Trial. “The use of OCS is actively expanding the donor pool, as I expected. It is time we stop considering heart transplant as a severely supply limited resource. With OCS we will be able to expand access to this life saving therapy to more end-stage heart failure patients.”
Schroder presented clinical trial results on Friday morning. The multicenter, randomized, U.S. Donation after Circulatory Death (DCD) trial utilized direct procurement and perfusion (DPP) with the Organ Care System (OCS). In this trial, patients awaiting heart transplantation were randomized in a three to one manner to a donation after circulatory death (DCD) eligible arm versus donation after brain death (DBD) only. Inclusion and exclusion criteria were pre-established both with regards to the recipient and donor characteristics but also with regards to the DCD management; for example, a functional warm ischemia time less than 30 minutes was defined and served as part of the trial protocol. This resulted in comparison of 80 DCD transplants versus 86 DBD cases, which were treated as randomized and per protocol. The DCD transplant cohort displayed significantly younger donor and recipient age. Furthermore, duration of wait list time was less for the DCD cohort. The primary effectiveness endpoint was patient survival at 6 months and did not differ between the two groups (95% DCD versus 89% DBD). Overall patient and graft survival at 2 years was significantly better in the DCD cohort (93%) versus the DBD control (83%). The incidence of moderate or severe LV or RV PGD was greater for the DCD group (22.5%) versus the DBD (9.5%).
This U.S. DCD trial was the first of its kind in that a randomized control group, deemed as DCD ineligible, was utilized and there were predetermined inclusion and exclusion criteria. The team concludes that despite higher rates of primary graft dysfunction, heart transplantation with DCD achieves intermediate survival outcomes equivalent to those achieved with DBD. Of note: Duke was the first and leading enroller in the trial.
In a note from Schroder to members of leadership this weekend, he reflected on the work:
“I am heading back from ISHLT in Boston after presenting the 2-year EXPAND heart and US DCD trials yesterday. Both ground breaking trials with results that have moved the needle in heart transplant. The DCD trial is probably the most meaningful thing to happen in heart transplant in the U.S. in many decades.
Now we, and anyone who is even remotely familiar with either trial, knows THAT THESE WERE REALLY DUKE TRIALS. We, as a team, made this happen out of sheer collective willpower.
Each and every team member should feel really great about this. Not only about the patients we helped along the way. But the countless more that will be helped in the future from our hard work.
I thank you all from the bottom of my heart for your efforts to continue to get the absolute best for Duke patients. And a special thanks to Sarah Casalinova who, for 6 years, has been the cornerstone to everything we have done with OCS.”
These results – the clinical trial findings, the FDA approval, the ISHLT presentations, and lives saved — stem from an incredible effort put forth over many years by members of this team. Their commitment to advanced heart failure patients with extremely limited options as well as their dedication to one another is truly inspiring. Congratulations!
And there is even more to celebrate from ISHLT:
 Duke Cardiology fellow Lauren Truby gave an excellent oral scientific presentation on “Proteomic profiling of cold storage preservation solution to identify signatures of primary graft dysfunction following heart transplantation.” This work helped to identify a set of novel biomarkers associated with primary graft dysfunction following heart transplantation; she also gave an excellent talk entitled, “Bridge to transplant with durable left ventricular assist device is associated with primary graft dysfunction: a report from the International Consortium on Primary Graft Dysfunction” and gave an invited presentation entitled “The rise of the machines: PGD risk scoring systems in the MCS bridge-to-transplant populations.” In summary: her work is helping to identify important clinical and biochemical risk factors for the development of primary graft dysfunction after heart transplantation.
Duke Cardiology fellow Lauren Truby gave an excellent oral scientific presentation on “Proteomic profiling of cold storage preservation solution to identify signatures of primary graft dysfunction following heart transplantation.” This work helped to identify a set of novel biomarkers associated with primary graft dysfunction following heart transplantation; she also gave an excellent talk entitled, “Bridge to transplant with durable left ventricular assist device is associated with primary graft dysfunction: a report from the International Consortium on Primary Graft Dysfunction” and gave an invited presentation entitled “The rise of the machines: PGD risk scoring systems in the MCS bridge-to-transplant populations.” In summary: her work is helping to identify important clinical and biochemical risk factors for the development of primary graft dysfunction after heart transplantation.
Way to go, Lauren!
 Duke cardiology fellow Vanessa Blumer was the only fellow invited to participate in and present during the first-ever, multi-national, ISHLT-endorsed Shock Consensus Conference. The focus was on identifying key areas of consensus for the care of patients with non-ischemic cardiogenic shock. She was asked to present a talk entitled, “How to proceed? Tools to quantify non-AMI cardiogenic shock severity and establish goals for treatment.”
Duke cardiology fellow Vanessa Blumer was the only fellow invited to participate in and present during the first-ever, multi-national, ISHLT-endorsed Shock Consensus Conference. The focus was on identifying key areas of consensus for the care of patients with non-ischemic cardiogenic shock. She was asked to present a talk entitled, “How to proceed? Tools to quantify non-AMI cardiogenic shock severity and establish goals for treatment.”
In summary: her contribution will hopefully lead to several consensus documents helping to identify priority areas for investigation focusing on the care of patients with cardiogenic shock unrelated to acute myocardial infarction.
ICYMI, Vanessa is co-author on a new perspectives piece Women Empowering Women in Heart Transplantation and Mechanical Circulatory Support that appears online (article in-press) in the Journal of Cardiac Failure.
Nicely done, Vanessa!
Chet Patel chaired a session entitled “Will you be mine? Choosing donors and recipients for heart transplantation” – Way to represent Duke Heart, Chet!
 Integrated thoracic surgery resident Julie Doberne presented on heart transplant in HIV-positive recipients and compared results with other solid organ transplants in same population. In a post to Twitter she credited Chet Patel and Carmelo Milano for being instrumental in the research and stated that HIV is no longer a death sentence.
Integrated thoracic surgery resident Julie Doberne presented on heart transplant in HIV-positive recipients and compared results with other solid organ transplants in same population. In a post to Twitter she credited Chet Patel and Carmelo Milano for being instrumental in the research and stated that HIV is no longer a death sentence.
Great work, Julie!
Comments from team members related to work presented at ISHLT include:
- “I’m extremely proud of all team member efforts leading the care of patients with cardiogenic shock, mechanical circulatory support, and heart transplantation.” – Jason Katz, Duke’s Director of Cardiovascular Critical Care; Co-Director, Duke Mechanical Circulatory Support Program, and Co-Director, Duke Cardiac Intensive Care Unit
- “Every day I am so thankful to have trained in HF at Duke but I’m especially proud today” – Amanda Coniglio via Twitter regarding Schroder presentations.
- “This is what it’s all about. JNS and our surgical team are the most fantastic surgeons out there-tireless, brilliant, committed, bringing real change to the field.” — Richa Agarwal via Twitter during Schroder presentations.
Heart Rhythm Society 2022, San Francisco
On the west coast this weekend, many of our Duke Heart faculty and fellows are attending and presenting during the Heart Rhythm Society 2022 annual meeting (April 29-May 1) in San Francisco.
 Earlier today, Jon Piccini presented 4-fold Higher Rate Of Atrial Fibrillation Detection After Stroke Of Presumed Known Etiology With Continuous Versus Intermittent Monitoring: Results From The Stroke AF Study:
Earlier today, Jon Piccini presented 4-fold Higher Rate Of Atrial Fibrillation Detection After Stroke Of Presumed Known Etiology With Continuous Versus Intermittent Monitoring: Results From The Stroke AF Study:
Despite progress in the prevention of stroke, it remains the fifth most common cause of death in the U.S. Atrial fibrillation increases the risk of stroke five-fold and is a common cause of stroke, especially in older individuals. Stroke often leads to permanent disability or death and identifying the cause of a stroke is an important step in preventing future or recurrent stroke.
Prior work has shown that between 20 and 30% of patients with stroke of undetermined cause (often referred to as cryptogenic stroke) have atrial fibrillation. Thus, patients with stroke of undetermined cause often undergo intensified heart rhythm monitoring in order to diagnose (and treat) atrial fibrillation as a potential cause of stroke. However, a recent analysis from the STROKE AF study suggests that looking for atrial fibrillation may be very important in patients whose stroke was not caused by atrial fibrillation and how we look for atrial fibrillation has important implications for providers and patients.
The STROKE AF study compared heart rhythm monitoring with an implantable cardiac monitor (ICM) versus standard approaches to intermittent heart rhythm monitoring in patients with stroke attributed to large artery atherosclerosis or small vessel occlusion. In patients whose stroke did not appear to be due to an abnormal heart rhythm, the study found that 1 in 8 patients had atrial fibrillation detected by an ICM by 12 months.
At today’s Heart Rhythm Society annual meeting, Piccini and colleagues reported on an additional analysis of the STROKE AF data.
In their analysis, they examined how the type of heart rhythm monitoring may impact the ability of monitoring to identify atrial fibrillation in these patients. As one might expect, they said, when comparing continuous monitoring with an ICM versus intermittent heart rhythm monitoring, continuous monitoring identified more instances of atrial fibrillation. However, and perhaps more importantly, even the most aggressive intermittent monitoring strategy would have missed 77% of patients with episodes of atrial fibrillation lasting an hour or more.
According to Piccini and team, these findings are important because after someone experiences a stroke, an important goal of care is to avoid another episode of stroke, no matter what caused the first. Individuals who have atrial fibrillation and a history of stroke have a Class I guideline recommendation for oral anticoagulation to prevent future stroke. The results from the STROKE AF investigators suggests that even with the most aggressive forms of intermittent monitoring, a large proportion of patients with atrial fibrillation would not be diagnosed and may go untreated.
“Traditionally, we have focused our efforts with AF screening in persons who had no clear cause of their stroke,” Dr. Jonathan Piccini, director of cardiac electrophysiology at Duke emphasized. “STROKE AF highlights the importance of diagnosing atrial fibrillation even in persons whose stroke appeared to be due to atherosclerosis or small vessel ischemia. Moreover, these data add to the growing evidence that highlight the importance of continuous cardiac monitoring in some patients who are at-risk for atrial fibrillation, regardless of what may have caused their first stroke.”
Great work, Jon!
Additional presentations during HRS included:
Duke cardiology fellow Kelly Arps presented Use Of Ripple Mapping To Enhance Localization And Ablation Of Outflow Tract  Premature Ventricular Contractions on Friday as well as a poster presentation Temporal Relationship Of Atrial Arrhythmias With The Diagnosis Of Cardiac Sarcoidosis.
Premature Ventricular Contractions on Friday as well as a poster presentation Temporal Relationship Of Atrial Arrhythmias With The Diagnosis Of Cardiac Sarcoidosis.
Jon Piccini presented Bridging the Gap in Guideline-driven Care for CIED Infections – We Must Do Better and Understanding the Clinical Utility of Anti-Tachycardia Pacing.
Marat Fudim presented Barostim: Patient Identification and Real World Experience during a session on Friday and Splanchnic Nerve Block in Heart Failure: Rationale and Clinical Application on Saturday.
Kevin Thomas co-chaired the Saturday session on Disparities or Differences in ICD/CRTD Utilization and earlier today co-chaired a session with Sana Al-Khatib on Racial and Ethnic Disparities in Clinical Electrophysiology.
Al-Khatib also served as a session commentator for Artificial Intelligence To Identify Left Ventricular Dysfunction From An Apple  Watch ECG: A Prospective, Decentralized International Pragmatic Study and presented Clinical Trials: Where does the Evidence Lie for Prevention of Pacing Induced Cardiomyopathy?
Watch ECG: A Prospective, Decentralized International Pragmatic Study and presented Clinical Trials: Where does the Evidence Lie for Prevention of Pacing Induced Cardiomyopathy?
Jim Daubert presented ICDs are No Longer Indicated for Primary Prevention in Patients with Non-ischemic Cardiomyopathy
Sean Pokorney presented Successes and Failures in Rhythm Control: Is it Time for a Hybrid Approach to Cardioversion, Ablation and AADs?
Impressive work by our Duke EP team. Way to go!!
ACTIV-3 Research Team Celebrated with Presidential Award
We are pleased to celebrate the Duke ACTIV-3 clinical research team, led by Peter K. Smith, MD — the team was presented with a Duke University Presidential Award for their continuing efforts in COVID-19 research on Wednesday, April 27 during a ceremony at Page Auditorium.

When Duke decided to halt all unnecessary clinical research activity at the start of the pandemic, Smith, the site PI for the Cardiothoracic Surgery Network (CTSN), recognized that the CTSN could be redirected for COVID-19 clinical trials due to how they were structured as well as their prior experience in the study of stem cells. The NIH quickly selected the CTSN to serve as one of four research platforms for the government’s unified response to COVID-19 – becoming the ACTIV-3 network. By mid-April 2020, Smith had not only gathered experts from throughout Duke Health to serve on the Duke-based ACTIV-3 clinical research team, the team had drafted the first clinical trial protocol using stem cell therapy for COVID-19 ICU patients.
With unprecedented speed and efficiency – the team created new infrastructure and established new systems to conduct COVID-19 research. Team members screened and consented patients 24/7/365, with staff working overtime, putting themselves and their families at potential risk at a time when very little was known about the virus. Multidisciplinary team capabilities were expanded, including pulmonary critical care physicians, infectious disease specialists, residents, and expansion from 4 to 32 clinical research staff dedicated to the project. Data and biospecimens were collected with an efficiency that far surpassed any that had previously been achieved in a clinical trial setting.
After completing the first stem cell study, the team then successfully helped to complete accrual to 5 other monoclonal antibody studies, one of which was recently published in the New England Journal of Medicine. The ACTIV-3 team currently has 2 other studies which are actively enrolling, including studies with new classes of promising therapeutics for the most critically ill patients. Almost 40% of patients enrolled at Duke have been African American, providing proportional representation of those most affected by COVID-19 in our community, which is something the ACTIV-3 team is especially proud of.

“We often don’t do a good job of enrolling the full breadth of our Duke patient population into clinical trials — meaning geographically, racially, ethnically and from a socio-economic standpoint, said Tom Holland, MD, a faculty member in infectious diseases. “The fact that we presented this to everybody, and we were willing to do the kinds of things to go to where patients were for follow up, for labs and visits to make it so that any patient who wanted to enroll, and was able to do so, could. We truly enrolled a population that looks a whole lot like the general population that we’ve taken care of for COVID.”
In 18 months, the ACTIV-3 international network enrolled more than 3000 patients across 139 sites, 422 of which have been accrued from Duke as the leading enrolling site, earning a special commendation from the Director of the NIH.
“This remarkable achievement is a testament to the commitment and dedication of the ACTIV-3 team which has shown single-minded purpose to save the lives of current and future patients most critically affected by the pandemic by enrolling them to clinical trials. We nominate the ACTIV-3 team for their courage and for serving as an inspiring example of what can be achieved through extraordinary teamwork,” states the team’s nomination letter.
“The surgery research group was very generous with their resources, making sure that we had clinical research coordinators and nurses to help get this going,” added Christina Barkauskas, MD, Duke faculty member in Pulmonary and Critical Care Medicine. “From the beginning we had a robust team that was willing to work hard, especially at the beginning of the pandemic when we felt like we had something different, novel and special to offer these patients – we wanted to give them the best chance we could, so we offered it to as many patients as we possibly could.”
nurses to help get this going,” added Christina Barkauskas, MD, Duke faculty member in Pulmonary and Critical Care Medicine. “From the beginning we had a robust team that was willing to work hard, especially at the beginning of the pandemic when we felt like we had something different, novel and special to offer these patients – we wanted to give them the best chance we could, so we offered it to as many patients as we possibly could.”
Speaking to Smith’s leadership of the ACTIV-3 team, Holland and Barkauskas were equally effusive.
“It was really fun to be able to experience his commitment to a project and to a mission and a scientific question — he has pretty remarkable drive,” Barkauskas said. “We knew what we wanted to do, and he would be persistent in finding a way to make it happen, and I think we all appreciated his constant presence to support the team. We screened patients every single day for two years. And getting this award is a nice testament to how hard we worked and how committed we all were. Sometimes it just feels good to get a little bit of recognition, even though we already felt good about what we were doing.”
Holland concurred, “Peter has been our captain and driving force for ACTIV-3 the whole time. He tends to deflect credit for this, but around the clock he was keeping an eye on who was coming into the hospital and who might be eligible for our trials. He was on every one of the calls multiple times a day to review what was going on. We would not have been able to keep up the pace of enrollment or maintain the motivation and vision to keep going as quickly as we did without his passion or his vision.”
Leading and working with the ACTIV-3 team has been refreshing, Smith says. “Seeing the capability of a multidisciplinary team that includes surgeons, experts from infectious disease, critical care, and the hospitalist program come together in this way has been exhilarating. This team created a potent research engine and it broke down a lot of the silos that can prevent certain kinds of research from thriving. I’m optimistic that we can branch out and potentially replicate this for further disease states.”
We are thrilled for the ACTIV-3 team – congratulations to all. The Presidential Award is well-deserved!
HCLC Sends Kudos to Duke Heart Team
The Spring Meeting of the Duke Heart Center Leadership Council (HCLC) took place on Friday, April 29 at the J.B. Duke Hotel & Conference Center in Durham.
The HCLC is led by Bob Keegan, who serves as Chair. The group heard overall highlights and updates from Manesh Patel and Ed Chen, co-directors of Duke Heart. Patel and Chen led a panel discussion, Focus on Discovery Science and Innovation with presentations by Chris Holley, Jennifer Rymer, Sreekanth Vemulapalli and Brittany Zwischenberger. Jill Engel presented an update on the efforts of our nursing and hospital-based teams during the pandemic as well as an update on cardiac nursing research.
The HCLC was truly impressed with the efforts reported on — particularly the care and dedication each and every Duke Heart team member exhibited during the pandemic.
Keegan and the HCLC requested that we specifically include a tremendous thanks to all employees across Duke Heart on their behalf in this weekend’s issue of Pulse. They asked us to send their profuse thanks for the incredible care we gave to patients coming to Duke Heart during the pandemic, for the advances we have been able to make despite the extreme challenges we faced because of the pandemic, the dedication all of us have shown by sticking together and standing by Duke Health, and for the care each of us takes in our respective positions — be they administrative, educational, research-focused, at the bench or at the bedside, they thank all of us for our work.
GREAT JOB, EVERYONE!
Shout-out to Duke Heart Administrative Professionals
A huge shout-out to our Duke Heart Administrative Professionals — they are some of the unsung heroes of healthcare, working behind the scenes to manage schedules, patient inquiries, appointments, paperwork — all “the things” (countless, really) that need doing to keep our faculty, fellows and other staff members organized and productive. Administrative Professionals Day was Wednesday, April 27, but it’s never too late to acknowledge their efforts and celebrate all they do.
Shout out to Holley

Our Ventricular Assist Device team wrote to us this week to recognize Chris Holley, MD, for the great rounding attending experience for their team during Patient Experience Week. Holley, often recognized for his research efforts as part of the Duke Cardiovascular Research Center, demonstrated his clinical excellence this week while leading the VAD clinical team for the LVAD service.
Comments from inpatient and outpatient APPs, fellows, pharmacists, nurses and patients recognize “his thoughtful attention and thorough evaluation of each issue with timely teaching moments for our fellows and other clinicians. His conversations with each patient and clinician on primary, outpatient and consult services represents the wisdom and kindness we hoped to inspire this week. Thanks Dr. Holley!”
Great job, Chris!
Duke Heart Global Efforts Celebrated in Magnify
Three of our terrific Duke Heart faculty members, Gerald Bloomfield, Waseem Akhter and Titus Ng’eno are featured in the current issue of Magnify, the Duke University School of Medicine magazine. The article, ‘A Pandemic in Slow Motion’: Duke Cardiologists Call for a New Approach to Prevent a Looming Global Crisis in Heart Health is a great way to learn more about the important work they are doing to advance access to cardiovascular care across the world. Inspiring!
Chen Featured in STS Podcast
Dr. Edward P. Chen, chief of the division of Cardiovascular and Thoracic Surgery is the featured guest in The Society of Thoracic Surgeons April 28 podcast (#133: Same Surgeon, Different Light: Dr. Ed Chen).
This is well worth a listen. Well done!
In Passing: Marc Caron, PhD, Professor of Cell Biology, Neurobiology and Medicine
We were saddened earlier this week by the passing of our long-time Duke colleague, Marc Caron, PhD, James B. Duke Professor of Cell Biology, Professor of Neurobiology and Professor of Medicine in Cardiology. Dr. Caron, 75, also was a member of the Duke Cancer Institute and Duke Institute for Brain Sciences.
of the Duke Cancer Institute and Duke Institute for Brain Sciences.
In a joint message from Mary Klotman, MD, Dean, Duke School of Medicine and Scott Soderling, PhD, Chair of the department of Cell Biology, they wrote:
An authoritative and prolific scientist, Dr. Caron spent all but two of his 47-year career at Duke. He studied the mechanisms of action and regulation of hormones and neurotransmitters and how they might underlie brain and behavior disorders such as schizophrenia, Parkinson’s disease, attention-deficit hyperactivity disorder, mood disorders and addiction. Among his many achievements, Dr. Caron and his colleagues engineered and characterized a large number of genetically modified mouse models to analyze the foundations of these various brain disorders. In a groundbreaking study, his team identified a novel mode of signaling for the brain’s dopamine D2 receptors, which are principal targets of antipsychotic medications. Dr. Caron also contributed to the discovery of how receptor signaling is regulated by kinases and arrestins, and he defined the molecular signals for their endocytosis and recycling as functional entities. His genetic gain and loss-of-function models provided evidence for the importance of GPCR regulation through kinases and arrestins and identified one of the first in vivo examples of G protein- versus arrestin-mediated GPCR signaling. Dr. Caron mentored many trainees, and followed them through their own careers with encouragement and advice.
Among his many honors, Dr. Caron was an investigator of the Howard Hughes Medical Institute from 1992 to 2004, a member of the American Academy of Arts & Sciences and a fellow of the American Association for the Advancement of Science. In 2005, he received the Julius Axelrod Award from the American Society for Pharmacology and Experimental Therapeutics. Dr. Caron authored more than 650 publications and served as editor or editorial board member of several leading journals including the Journal of Clinical Investigation.
Dr. Caron received his BSc in Chemistry from Laval University and his PhD from the University of Miami. He completed a postdoctoral fellowship at Duke University. He joined the faculty of Laval University School of Medicine as an assistant professor in 1975, and then returned to join Duke’s faculty in 1977.
His funeral mass was held yesterday at Immaculate Conception Catholic Church in Durham. An online obituary can be found here.
Our deep condolences go out to Dr. Caron’s family, friends and his colleagues throughout the world.
COVID-19 Update
All the latest Clinical Operations updates related to COVID can be found at https://covid-19.dukehealth.org. Patient-facing resources on DukeHealth.org can be found here: https://www.dukehealth.org/covid-19-update/resources. Duke University maintains a resource page as well, which can be accessed here: https://coronavirus.duke.edu/updates/for-staff.
Upcoming Events & Opportunities
Cardiology Grand Rounds
May 3: Precision Medicine in Arrhythmias: Not Your Daddy’s Long QT with Navid Nafissi. 5 p.m. Webex.
May 10: Coronary CTOs and Cardiac MRI: The Duke Experience with Caitlin Dresher. 5 p.m., Webex.
MDEpiNet Spring 2022 Virtual Mini-Think Tank
May 5: MDEpiNet Spring 2022 Virtual Mini-Think Tank. Noon – 5:30 p.m., ET
MDEpiNet Predictable And SuStainable Implementation Of National CardioVascular Registries (PASSION CVR) Registry-Supported Prospective Clinical Trials
Join and invite your colleagues to join for updates from, and dialogues across our Registry-supported Prospective Trials Working Groups:
- Data Governance & Access
- Operational Roles & Responsibilities
- Global Regulatory Acceptance
- Use Cases:
- Aortic Intervention
- Heart Valves
- Mechanical Circulatory Support
- Peripheral Arterial Intervention
Registration now open: https://duke.qualtrics.com/jfe/form/SV_2f6JBD6WfaF9jBc.
Evening with Heart Raleigh
An Evening with Heart Raleigh, which has been rescheduled from earlier this year, will benefit Marfan families as well as those with Loeys-Dietz (LDS), Vascular Ehlers-Danlos (VEDS), and related conditions.
May 5, 2022
The Maxwell
7-10 p.m.
Cocktail attire
Tickets for the event include open bar, taco bar, heavy appetizers, dessert, silent auction, DJ, and a fun photo booth. For those unable to attend in person but who would like to participate, the silent auction items can be bid on online from anywhere. Lots of cool items have been donated so far! For tickets, more information or silent auction viewing and bidding, please visit: https://marfan.ejoinme.org/raleigh22.
Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged. Submissions by Noon, Wednesdays, to be considered for weekend inclusion.
Duke Heart in the News:
April 25 — Stuart Knechtle (transplant surgery)
CBS17.com
NC mom, daughter share organ transplant journey during National Donate Life Month
https://duke.is/m4tqy
April 26 — Gerald Bloomfield
Poz.com
More Cardiac Abnormalities Seen in People Living With HIV
https://duke.is/2byb2
April 27 — Duke University Health System
Becker’s Hospital Review
36 hospitals on Forbes list of best employers for diversity
https://duke.is/gyqpy
April 27 — Joe Turek
CBS News/CBS Mornings
First-of-its-kind heart transplant in infant could possibly prevent organ rejection
https://duke.is/zfek5
April 28 — Manesh Patel
Healio/Cardiology
Asundexian confers lower bleeding rates vs. apixaban for stroke prevention in AF
Division of Cardiology Publications Indexed in PubMed April 21-27, 2022
Ani C, Shavlik D, Knutsen S, Abudayyeh I, Banta J, O’Brien E, Mentz RJ, Bertoni AG, Fraser G. Glycemic status, non-traditional risk and left ventricular structure and function in the Jackson Heart Study. BMC Cardiovasc Disord 2022 Apr 21;22(1):186. PM: 35448969.
Berkowitz SD, Bauersachs RM, Szarek M, Nehler MR, Debus ES, Patel MR, Anand SS, Capell WH, Hess CN, Hsia J, Leeper NJ, Brasil D, Mátyás L, Diaz R, Brodmann M, Muehlhofer E, Haskell LP, Bonaca MP. Prevention of arterial and venous thrombotic events in symptomatic peripheral arterial disease patients after lower extremity revascularization in the VOYAGER PAD trial: Dual anticoagulant/antiplatelet regimen vs antiplatelet therapy alone. J Thromb Haemost 2022 May;20(5):1193-1205. PM: 35170216.
Coniglio AC, Mentz RJ. Sleep Breathing Disorders in Heart Failure. Cardiol Clin 2022 May;40(2):183-189. PM: 35465892.
Cooper-DeHoff RM, Niemi M, Ramsey LB, Luzum JA, Tarkiainen EK, Straka RJ, Gong L, Tuteja S, Wilke RA, Wadelius M, Larson EA, Roden DM, Klein TE, Yee SW, Krauss RM, Turner RM, Palaniappan L, Gaedigk A, Giacomini KM, Caudle KE, Voora D. The Clinical Pharmacogenetics Implementation Consortium Guideline for SLCO1B1, ABCG2, and CYP2C9 genotypes and Statin-Associated Musculoskeletal Symptoms. Clin Pharmacol Ther 2022 May;111(5):1007-1021. PM: 35152405.
Goodney P, Shah S, Hu YD, Suckow B, Kinlay S, Armstrong DG, Geraghty P, Patterson M, Menard M, Patel MR, Conte MS. A systematic review of patient-reported outcome measures patients with chronic limb-threatening ischemia. J Vasc Surg 2022 May;75(5):1762-1775. PM: 35085747.
Greene SJ, Tan X, Yeh YC, Bernauer M, Zaidi O, Yang M, Butler J. Factors associated with non-use and sub-target dosing of medical therapy for heart failure with reduced ejection fraction. Heart Fail Rev 2022 May;27(3):741-753. PM: 33471236.
Mark DB, Spertus JA, Bigelow R, Anderson S, Daniels MR, Anstrom KJ, Baloch KN, Cohen DJ, Held C, Goodman SG, Bangalore S, Cyr D, Reynolds HR, Alexander KP, Rosenberg Y, Stone GW, Maron DJ, Hochman JS. Comprehensive Quality-of-Life Outcomes With Invasive Versus Conservative Management of Chronic Coronary Disease in ISCHEMIA. Circulation 2022 Apr 26;145(17):1294-1307. PM: 35259918.
Minhas AMK, Salah HM, Khan MS, Rao VN, Tedford RJ, Reddy YNV, Caughey MC, Savarese G, Greene SJ, Michos ED, Fudim M. Most Common Causes of Hospitalization Associated with Inpatient Mortality in the United States Between 2005-2018. Am J Med Sci 2022 May;363(5):459-461. PM: 35090870.
Simonato M, Vemulapalli S, Ben-Yehuda O, Wu C, Wood L, Popma J, Feldman T, Krohn C, Hardy KM, Guibone K, Christensen B, Alu MC, Chen S, Ng VG, Chau KH, Shahim B, Vincent F, MacMahon J, James S, Mack M, Leon MB, Thourani VH, Carroll J, Krucoff M. Minimum Core Data Elements for Evaluation of TAVR: A Scientific Statement by PASSION CV, HVC, and TVT Registry. Ann Thorac Surg 2022 May;113(5):1730-1742. PM: 35367049.
Singh AK, Blackorby A, Cizman B, Carroll K, Cobitz AR, Davies R, Jha V, Johansen KL, Lopes RD, Kler L, Macdougall IC, McMurray JJV, Meadowcroft AM, Obrador GT, Perkovic V, Solomon S, Wanner C, Waikar SS, Wheeler DC, Wiecek A. Study design and baseline characteristics of patients on dialysis in the ASCEND-D trial. Nephrol Dial Transplant 2022 Apr 25;37(5):960-972. PM: 33744933.
Smilowitz NR, Cornwell M, Offerman EJ, Rockman CB, Shah SH, Newman JD, Ruggles K, Voora D, Berger JS. Risk factors, transcriptomics, and outcomes of myocardial injury following lower extremity revascularization. Sci Rep 2022 Apr 25;12(1):6718. PM: 35468922.
Voora D, Baye J, McDermaid A, Narayana Gowda S, Wilke RA, Nicole Myrmoe A, Hajek C, Larson EA. SLCO1B1*5 Allele Is Associated With Atorvastatin Discontinuation and Adverse Muscle Symptoms in the Context of Routine Care. Clin Pharmacol Ther 2022 May;111(5):1075-1083. PM: 35034348.
White HD, Schwartz GG, Szarek M, Bhatt DL, Bittner VA, Chiang CE, Diaz R, Goodman SG, Jukema JW, Loy M, Pagidipati N, Pordy R, Ristić AD, Zeiher AM, Wojdyla DM, Steg PG. Alirocumab after acute coronary syndrome in patients with a history of heart failure. Eur Heart J 2022 Apr 19;43(16):1554-1565. PM: 34922353.
Recent Comments