Duke Heart Pulse week ending July25th 2021
Highlights of the week:
Duke CTS among Top 20 for TSF Funding
The Thoracic Surgery Foundation (TSF) this week announced its “Top 20” Institutional Honor Roll for 2021. Duke University’s Cardiovascular & Thoracic surgical team ranked at #18 with a total of $365,000 in grant funding received.
TSF, which is the charitable arm of The Society of Thoracic Surgeons (STS), provides awards for cardiothoracic surgery research, education, leadership, and surgical outreach in underserved patients. So far in 2021, the Foundation has distributed $861,870 in awards and scholarships. The Foundation plans to award additional grants later in the year.
“Pursuit of the academic mission is deeply entrenched throughout the fabric of this institution,” said Edward P. Chen, MD, chief of Duke’s Division of Cardiovascular and Thoracic Surgery. “Being in the TSF Top 20 Institutional Honor Roll is reflective of not only our Division’s longstanding commitment to scientific discovery and academic development, but is also a testament to the longevity of this commitment.”
The TSF “Top 20” most funded institutions since 1993 are:
#1 University of Pittsburgh
#2 University of Pennsylvania
#3 Washington University
#4 University of California San Francisco
#5 Johns Hopkins Hospital
#6 University of Virginia
#7 University of Washington
#8 Tie – University of California Los Angeles
#8 Tie – Stanford University
#10 University of Michigan
#11 Massachusetts General Hospital
#12 Brigham and Women’s Hospital
#13 University of Toronto
#14 University of Colorado
#15 Baylor College of Medicine
#16 Medical College of Wisconsin
#17 University of Cincinnati
#18 Duke University
#19 Roswell Park Cancer Center
#20 Northwestern Memorial Hospital
“We congratulate each of these institutions for achieving TSF Top 20 Honor Roll status. This status signals the strength of their cardiothoracic surgery programs, faculty, and staff,” said TSF President Joseph E. Bavaria, MD. “Each TSF funding application is thoroughly analyzed and scored by rigorous peer review, without bias or conflict of interest. The TSF Research Committee is composed of more than 46 appointed surgeon-scientist leaders who are actively practicing at medical institutions across the U.S. and Canada. The contributions of award recipients at these Top 20 institutions to cardiothoracic surgery and our patients is significant.”
The Foundation’s 2022 Award cycle launched on July 1, 2021. TSF welcomes applications from qualified cardiothoracic surgeons and residents, employed at any institution with a cardiothoracic surgery program. Award offerings and applications can be accessed at www.thoracicsurgeryfoundation.org/awards. The deadline for most TSF Award applications is September 15, 2021.
Congratulations to all members of our Division of Cardiovascular and Thoracic Surgery on this great accomplishment!
Blumer Selected as Laennec Finalist
 Vanessa Blumer, MD, has been selected by the American Heart Association’s Council on Clinical Cardiology (CLCD) as a finalist for the 2021 Laennec Fellow in Training (FIT) Clinician Award Competition!
Vanessa Blumer, MD, has been selected by the American Heart Association’s Council on Clinical Cardiology (CLCD) as a finalist for the 2021 Laennec Fellow in Training (FIT) Clinician Award Competition!
The Laennec FIT Clinician Award recognizes the importance of clinical acumen, inductive analytic skills, and teaching ability in future academic cardiologists; it is a highly competitive award category.
Blumer, a third year fellow in our cardiovascular disease fellowship program, will present her abstract, A Challenging Case of Endocarditis — Multi-Disciplinary Approach is an Achievable Chimera during the Laennec FIT Award Competition Session at the upcoming AHA Scientific Sessions scheduled for November 13-15, 2021, in Boston, MA.
Outstanding! Congratulations, Vanessa!
Kudos to Yankey!
This week, we received the following note regarding excellent care and attention provided by Sipa Yankey and team to a patient and their family members at the Durham VAMC.
and their family members at the Durham VAMC.
“Dr. Rao,
This email is to let you know my husband’s comments concerning Doctor Yankey’s diagnosis and treatment for him in Durham VA hospital.
[He] has not been feeling well for some time now and I had been trying to get him to a heart doctor. Once he visited the VA in Salisbury to see Doctor Card, she immediately scheduled him to be seen and treated in Durham. Once we arrived at Durham VA we could see the great care offered to all veterans. The staff is so very professional and caring, especially Doctor Yankey. He installed a stent in the LAD in [my husband’s] heart which was 99 percent blocked. He SAVED his life! And he was so calm as he explained, in detail, what he had to do to correct his problem. He had a nurse by the name of Kim, not sure of last name, but she was excellent also and very detailed on explaining what all the steps would be to give comfort to my wife and daughters. She took the time to answer questions as also Doctor Yankey did to our daughter that is a registered nurse. Kim has a husband that also worked in one of the areas that called to check on him when he arrived home. What great staff and so caring.
We realize you may not always get appreciation shown for your staff. We feel it is important to let you know that with God’s help and the great knowledge and skills that Doctor Yankey has is what saved [my husband]’s life.
Doctor Yankey diagnosed and operated on [my husband] and did an excellent job! How do you thank someone that saves your life?
Again, we both wanted to show appreciation for the care and expert skills that you provide to our veterans who protect our country.
Thank you.” — Name withheld to protect patient privacy
Way to go, Sipa!
Duke Raleigh Hospital Names New President
 Barbara Griffith, MD, will be returning to Duke Health to become president of Duke Raleigh Hospital.
Barbara Griffith, MD, will be returning to Duke Health to become president of Duke Raleigh Hospital.
Griffith, who currently serves as president and chief executive officer of Woman’s Hospital in Baton Rouge, La., had previously been at Duke Regional Hospital as Chief Medical Officer and president and chief financial officer of Durham Emergency Physicians, the medical practice within Duke Regional Hospital’s emergency department.
“Duke Health and North Carolina have always been home,” Griffith said. “It is such a privilege to join the amazing team at Duke Raleigh Hospital when it is growing its footprint in Wake County and opening a beautiful new bed tower, the South Pavilion. I am thrilled that I will soon be a part of it.”
Griffith received her medical degree at the University of North Carolina at Chapel Hill. She is board certified in emergency medicine and has received training in executive health care education at the Wharton School of Business.
“Dr. Griffith joins us at a critical time when the health system is growing to deliver care to the many thousands of patients who seek out the quality care that we provide,” said William J. Fulkerson, Jr., MD, executive vice president of Duke University Health System. “Her experience as a leader in safety and quality and as a highly regarded physician whom our providers and staff trust make her a remarkable fit for this role.”
During the year-long recruitment process, Leigh Bleecker served as interim president of Duke Raleigh Hospital and will return to her role as chief financial officer.
REMINDER: Change Passwords to Comply with New Policy
Duke Health users and sponsored guests must update passwords as soon as possible, but will not be required to change passwords in the future – unless you want to update it or your password is compromised.
The new password policy removes the requirement to update passwords every 180 days and requires passwords to be at least 12 characters (special characters and numbers are no longer required); however, including special characters creates a stronger password. In addition, the option to update passwords using CTRL+ALT+DEL is no longer available.
Team members can update their passwords now, but will receive a notice from DHTS via email that requires passwords to be changed by a deadline. Please visit the OIT Account Self Service Portal and create a new NetID password that doesn’t expire.
Tip: If working remotely (at a non-Duke site) users should connect to the Duke Virtual Private Network (VPN) before updating passwords (see page 29 of the Technology Toolkit for more information about the VPN). Passwords can be updated without connecting to the VPN, but passwords are synced across all your Duke log-ins faster if connected to the VPN.
Visit https://security.duke.edu/news-alerts/new-password-policy to review the password policy FAQ.
Attention Omnicell Users
Due to Omnicell’s password policy, Duke Health employees that use Omnicell, with the exception of Duke Raleigh Hospital employees, must keep passwords to 15 characters or less; Duke Raleigh Hospital employees must keep passwords to a maximum of 30 characters.
We are working with Omnicell to upgrade their password policy to remove restrictions across Duke Health. Check the password policy information page for updates.
Contact the Duke Health Service Desk at (919) 684-2243 for technical support.
If you have not yet updated your passcode to fit this policy, please do so as soon as possible. Thank you!
Upcoming Events/Opportunities
Conversations with Colleagues expands offerings
The Conversations with Colleagues program has changed the way we talk with one another about tough topics like COVID-19 and racial justice. Now the team is adding two additional timely topics to the mix, as well as opening up another cohort of their highly popular extended series that takes a deeper dive into racial justice. Deeper Dive and Returning to the Workplace are open to all Duke Health team members, while The Social Side of Medicine is for clinical professionals and PFAC members. Learn more and sign up below.
Racial Justice: Deeper Dive
This six-week transformative experience explores the origins of systemic racism and helps participants understand their own implicit biases and what they can do to have a positive impact on our local community. The curriculum includes mixed media to engage all learning styles. Because this is a cohort-based experience based on building relationships, we ask that attendees commit to all six weeks of the series. You will select a day and time that works for you and will be expected to attend all six sessions on that set day. Sign up for a cohort to start in August:
Wednesdays from 8-9am
https://duke.zoom.us/meeting/register/tJYtfu2oqDIpHtMLUx6L2EZim8Ldd1RjOiaC
Fridays from 12-1pm
https://duke.zoom.us/meeting/register/tJwvceyvqz4qHdLjVhx-HDSt6_Aj835UDN_1
New Topic: Returning to the Workplace
Many teams are transitioning back to the office after a long period of working from home. As with any change, this transition can invoke a flurry of different emotions. Your CwC friends are here to talk through this transition with you. Please join us at any of the sessions listed below. Sign up here: https://bit.ly/dukecwc
Wednesday 8/11 8 a.m.
Wednesday 8/11 12 noon
Friday 8/13 at 12 noon
For Clinical Professionals and PFAC Council Members: The Social Side of Medicine
Patient and Family Engagement (PFE) and Conversations with Colleagues are excited to offer a different kind of conversation. We invite clinical professionals of all disciplines and Patient and Family Advisors (PFAs) who serve on one of Duke Health’s 10 Patient and Family Advisory Councils to come together and discuss the “Social Side of Medicine.” During this guided, hour-long conversation, we will explore communication between patients and clinical professionals, how we can build stronger partnerships, and how we can continually improve the quality and delivery of care. Sign up here: https://bit.ly/dukecwc
Wednesday 7/28, 6pm
Friday 7/30, 12 noon
Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged.
Duke Heart in the News:
July 19 — Duke University Hospital
Healio
Top in cardiology: Next-generation artificial heart, methamphetamine-related heart failure
http://duke.is/Mn3FSY
July 20 — Carmelo Milano
Interesting Engineering
First Total Artificial Heart Successfully Transplanted In the US
http://duke.is/bSLrGq
July 20 — Carmelo Milano
Republic World
French Prosthetics Company Carmat Makes First-ever Commercial Sale Of Artificial Heart
http://duke.is/kiGytc
July 20 — Robert Califf
Infection Control Today
COVID-19 Isn’t Done with Us Yet, Medical Experts Warn
http://duke.is/VbDuxR
July 20 — Duke University Hospital
QMED New Product News
First US Implant of Carmat’s Total Artificial Heart Performed at Duke
http://duke.is/mCRfT6
*story carried in 17 other news outlets
July 20 — Stephen Greene and Muhammad Shahzeb Khan
Healio/Cardiology Today
Lung ultrasound in ED to manage acute HF confers no benefit vs. usual care
http://duke.is/gm8Ebz
July 20 — Carmelo Milano
Home Healthcare Business News
Duke implants first new generation artificial heart in North America
https://www.dotmed.com/news/story/55378
July 21 — Carmelo Milano and Jacob Schroder
Insider.com
http://duke.is/kabNC6
July 21 — Duke University Hospital
WTRF.com (Wheeling, WV)
U.S patient gets first total artificial heart implant
http://duke.is/nId6CE
July 21 — Carmelo Milano and Jacob Schroder
Plastics Today
Transatlantic Milestones for Carmat’s Total Artificial Heart
Division of Cardiology Publications Indexed in PubMed July 15-21, 2021
Amin AP, Rao SV, Seto AH, Thangam M, Bach RG, Pancholy S, Gilchrist IC, Kaul P, Shah B, Cohen MG, Gluckman TJ, Bortnick A, DeVries JT, Kulkarni H, Masoudi FA. Transradial Access for High-Risk Percutaneous Coronary Intervention: Implications of the Risk-Treatment Paradox. Circ Cardiovasc Interv. 2021;14(7):e009328. PM: 34253050.
Biering-Sørensen T, Minamisawa M, Liu J, Claggett B, Papolos AI, Felker GM, McMurray JJV, Legg JC, Malik FI, Honarpour N, Kurtz CE, Teerlink JR, Solomon SD. The effect of the cardiac myosin activator, omecamtiv mecarbil, on right ventricular structure and function in chronic systolic heart failure (COSMIC-HF). Eur J Heart Fail 2021;23(6):1052-1056. PM: 33826209.
Desai ND, O’Brien SM, Cohen DJ, Carroll J, Vemulapalli S, Arnold SV, Forrest JK, Thourani VH, Kirtane AJ, O’Neil B, Manandhar P, Shahian DM, Badhwar V, Bavaria JE. Composite Metric for Benchmarking Site Performance in Transcatheter Aortic Valve Replacement: Results From the STS/ACC TVT Registry. Circulation 2021;144(3):186-194. PM: 33947202.
Gilotra NA, Pamboukian SV, Mountis M, Robinson SW, Kittleson M, Shah KB, Forde-McLean RC, Haas DC, Horstmanshof DA, Jorde UP, Russell SD, Taddei-Peters WC, Jeffries N, Khalatbari S, Spino CA, Richards B, Yosef M, Mann DL, Stewart GC, Aaronson KD, Grady KL. Caregiver Health-Related Quality of Life, Burden, and Patient Outcomes in Ambulatory Advanced Heart Failure: A Report From REVIVAL. J Am Heart Assoc 2021;10(14):e019901. PM: 34250813.
Giroux NS, Ding S, McClain MT, Burke TW, Petzold E, Chung HA, Palomino GR, Wang E, Xi R, Bose S, Rotstein T, Nicholson BP, Chen T, Henao R, Sempowski GD, Denny TN, Ko ER, Ginsburg GS, Kraft BD, Tsalik EL, Woods CW, Shen X. Chromatin remodeling in peripheral blood cells reflects COVID-19 symptom severity. bioRxiv 2020:2020.12.04.412155. PM: 33300002.
Goldsweig AM, Povsic TJ. Complex Percutaneous Coronary Intervention: Discrete Entity or Just Another Subgroup to Analyze? Circ Cardiovasc Interv 2021;14(7):e010891. PM: 34130479.
Haga SB, Mills R, Moaddeb J, Liu Y, Voora D. Delivery of Pharmacogenetic Testing with or without Medication Therapy Management in a Community Pharmacy Setting. Pharmgenomics Pers Med 2021;14:785-796. PM: 34276225.
Hiatt WR, Hess CN, Bonaca MP, Kavanagh S, Patel MR, Baumgartner I, Berger JS, Blomster JI, Jones WS, Katona BG, Mahaffey KW, Norgren L, Rockhold FW, Fowkes FGR. Ankle-Brachial Index for Risk Stratification in Patients With Symptomatic Peripheral Artery Disease With and Without Prior Lower Extremity Revascularization: Observations From the EUCLID Trial. Circ Cardiovasc Interv 2021;14(7):e009871. PM: 34253048.
Jering KS, Claggett B, Pfeffer MA, Granger C, Køber L, Lewis EF, Maggioni AP, Mann D, McMurray JJV, Rouleau JL, Solomon SD, Steg PG, van der Meer P, Wernsing M, Carter K, Guo W, Zhou Y, Lefkowitz M, Gong J, Wang Y, Merkely B, Macin SM, Shah U, Nicolau JC, Braunwald E. Prospective ARNI vs. ACE inhibitor trial to DetermIne Superiority in reducing heart failure Events after Myocardial Infarction (PARADISE-MI): design and baseline characteristics. Eur J Heart Fail 2021;23(6):1040-1048. PM: 33847047.
Khan MS, Fonarow GC, Greene SJ. Sodium-glucose co-transporter 2 inhibitors for heart failure: clinical trial efficacy and clinical practice effectiveness. Eur J Heart Fail 2021;23(6):1023-1025. PM: 33779013.
Khan MS, Sreenivasan J, Shahid I, Bhinder J, Fudim M, Greene SJ, Butler J. Trends in Substance Abuse Disorders Among Patients Hospitalized for Heart Failure in the United States. Circ Heart Fail 2021;14(7):e008147. PM: 34233481.
Kitzman DW, Whellan DJ, Duncan P, Pastva AM, Mentz RJ, Reeves GR, Nelson MB, Chen H, Upadhya B, Reed SD, Espeland MA, Hewston L, O’Connor CM. Physical Rehabilitation for Older Patients Hospitalized for Heart Failure. N Engl J Med 2021;385(3):203-216. PM: 33999544.
Kochar A, Summers MB, Benziger CP, Marquis- Gravel G, DeWalt DA, Pepine CJ, Gupta K, Bradley SM, Dodson JA, Lampert BC, Robertson H, Polonsky TS, Jones WS, Effron MB. Clinician engagement in the ADAPTABLE (Aspirin Dosing: A Patient-centric Trial Assessing Benefits and Long-Term Effectiveness) trial. Clin Trials 2021;18(4):449-456. PM: 33541120.
Matos JD, McIlvaine S, Grau-Sepulveda M, Jawitz OK, Brennan JM, Khabbaz KR, Sellke FW, Yeh R, Zimetbaum P. Anticoagulation and amiodarone for new atrial fibrillation after coronary artery bypass grafting: Prescription patterns and 30-day outcomes in the United States and Canada. J Thorac Cardiovasc Surg 2021;162(2):616-624. PM: 32197901.
O’Brien EC, Raman SR, Ellis A, Hammill BG, Berdan LG, Rorick T, Janmohamed S, Lampron Z, Hernandez AF, Curtis LH. The use of electronic health records for recruitment in clinical trials: a mixed methods analysis of the Harmony Outcomes Electronic Health Record Ancillary Study. Trials 2021;22(1):465. PM: 34281607.
Rao VN, Bush CG, Mongraw-Chaffin M, Hall ME, Clark D, Fudim M, Correa A, Hammill BG, O’Brien E, Min YI, Mentz RJ. Regional Adiposity and Risk of Heart Failure and Mortality: The Jackson Heart Study. J Am Heart Assoc 2021;10(14):e020920. PM: 34238024.
Roe MT, Patrick-Lake B, von Eschenbach AC. Post-COVID-19 Syndrome: Leveraging the Patient Perspective and Technological Innovations to Enable the Delineation of Effective Treatments. Drugs 2021;81(10):1235-1237. PM: 34132992.
Duke Heart Pulse Week ending 7-18-2021
Highlights of the week:
New Generation Artificial Heart Implanted in Patient at Duke – First in U.S.
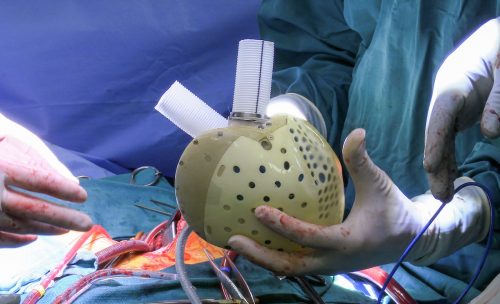
A surgical team at Duke University Hospital, led by Drs. Jacob Schroder and Carmelo Milano, successfully implanted a new-generation artificial heart in a 39-year-old man with heart failure, becoming the first center in North America to perform the procedure.


The artificial heart was developed by CARMAT and has been studied in Europe, where it is approved for use. Last year, the company received FDA approval to begin studies in the U.S. to potentially enroll 10 patients with end-stage bi-ventricular heart failure. The study will evaluate whether the artificial heart is a viable option as a life-saving step before transplant.
“We are encouraged that our patient is doing so well after the procedure Monday,” said Milano, a transplant surgeon and the principal investigator of the device study at Duke. “As we evaluate this device, we are both excited and hopeful that patients who otherwise have few to no options could have a lifeline.”
The Duke patient, Matthew Moore, is from Shallotte, N.C., and was referred to Duke in June after a sudden, unexpected diagnosis of heart failure. Moore and his wife, Rachel, recently adopted their two-year-old foster son, Marshall, and arrived at Duke expecting only to undergo heart bypass surgery.
As Moore’s condition quickly deteriorated, however, traditional options, including transplant, became too risky. Meanwhile, Duke was among just three transplant centers in the United States selected to join the device study, and the procedure team received specialized training to prepare for the implant surgery.
“As a nurse, I understand how important it is to bring these advancements forward,” Rachel Moore said. “Both Matthew and I are so grateful that we’ve been provided an opportunity to participate in something that has the potential to have an impact on so many lives. We are just taking it day-by-day and hope everything continues to progress well.”
The artificial heart developed by CARMAT is an implantable prosthetic that includes biological valves derived from bovine tissue. It operates on an external power supply.
If the device receives FDA approval, it would provide a bridge to transplant for patients whose hearts require assistance to pump blood through both chambers. Current technology – notably a left-ventricular assist device (LVAD) — supports just one chamber.
“Because of the shortages of donor hearts, many patients die while waiting for a heart transplant,” said Schroder, a transplant surgeon who led the implant procedure. “We are hopeful for new options to help these patients, many like Mr. Moore who have devastating disease and cannot otherwise be considered for a transplant.”
Manesh Patel, M.D., chief of the Division of Cardiology in Duke’s Department of Medicine, said the heart care program at Duke has fostered a culture of innovation over decades, aimed at improving care for patients.
“Our goal is to both deliver the best health care and to play a role in discovering it,” Patel said. “Innovation is essential for this. Patients locally and nationally are seen by our heart transplant team for care they may not get elsewhere. The key is the culture of innovation and the teamwork between our cardiac surgeons, heart failure cardiologists, nurses and all the heart center staff that care for our patients.”

Dr. Jason Katz, co-director of Duke’s Mechanical Circulatory Support Program and co-PI on the CARMAT trial agrees, “This is another example of multidisciplinary collaborative innovation for our advanced heart failure patients and speaks to how important innovation of patient care is to the entire team. It’s the first of what I hope will be many innovative options for this high risk patient population.”
Clinical research nurse coordinator for the trial, Frank Benedetti added, “A million things had to happen over the past several weeks, but all the pieces fell in line. When I got the call that the patient was out of the OR and had done well, I teared up with joy. It was such a proud moment to see all of our hard work come together and really pay off for this patient – I am so proud of our whole team.”
“The successful implant of the CARMAT artificial heart represents the latest in a long list of accomplishments by the Duke heart transplant team aimed at further expanding the treatment options available for patients with end-stage cardiac disease,” said Edward P. Chen, M.D., chief of the Division of Cardiovascular and Thoracic Surgery in Duke’s Department of Surgery.
Many thanks to our cardiothoracic surgical team led by Drs. Jacob Schroder and Carmelo Milano; to our Cardiac

Anesthesiology team members, Drs. Sharon McCartney, Alina Nicoara, Meredith Whitacre and Mihai Podgoreanu; all of our VAD coordinators, Laura Blue, Kevin Cox, Catherine Shuford, Dakota Bentz; our perfusion team; the entire nursing staff of the CTICU and clinical stepdown unit teams, including the Advance Practice Providers who are getting very familiar with a device that no other APP team in the U.S. is familiar with; and our Clinical Research Team, especially our clinical research nurse coordinator Frank Benedetti, “who was asked to do a lot on a very short timeline and came through with flying colors,” said Katz. We also thank the CICU who help care for the patient during his course of illness and kept him stable and supported to get to the CT surgical team.
Benedetti acknowledged the help of dozens of people including Robyn Osborne, laboratory manager at Substrate Services Core Research Support team in the Department of Surgery; Susan Churchill with the Multi-Dimensional Image Processing Laboratory in Duke Radiology, Brian Gore with Duke University Hospital Clinical Engineering; Diane Pinder, a fellow clinical research nurse coordinator, and Clancy Leahy, research project manager with SOCR.
A Duke press conference to discuss the device was held on Thursday afternoon. A link to the recording can be found here: https://youtu.be/GAI22Y6ksjo.
Shout-out to Barba & Team!
We received a recognition note this past week from Diane Sauro, director – Advanced Practice, for Ashley Barba and members of the patient care team.
“Ashley, see below comment from report I received from Patient Visitor Relations. The awesome, compassionate care you provide to your patients does not go unnoticed. You are a role model to your team. Thank you for everything you do for Heart patients and your team.” —Diane
“Patient complimented Dezarae, Sonya, Taylor, Kaitlyn, Samantha, Ashley and Kat. Patient stated, “They were outstanding nurses!!! They were always attentive and very responsive. They listened to me and answered all of my questions in ways that I could understand. Most importantly they always treated me as a person and not just a patient!”
Great job, everyone!
Upcoming Events/Opportunities
July 20: COVID-19 Research Seminar Series featuring Christina Barkauskas and Manesh Patel. 4-5 p.m. Zoom. Sponsored by Duke University School of Medicine.

Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged.
Duke Heart in the News:
July 9 — Duke Clinical Research Institute
Becker’s Health IT
8 hospitals, health systems that launched innovation centers in 2021
https://bit.ly/3Bea92R
July 14 — Duke University Medical Center
Rev Cycle Intelligence
Study Raises Concerns About Gender Pay Gap in Healthcare
https://bit.ly/3BgtnoE
July 15 — Carmelo Milano and Jacob Schroder
WRAL/NBC-5
Adoptive father of 2-year-old becomes first patient to get artificial heart at Duke
https://bit.ly/3BhwQTJ
July 15 — Duke University Hospital
Nuevo Periodico
La empresa francesa Carmat realiza la primera implantación humana de su corazón artificial total
https://bit.ly/3rhlIln
July 15 — Carmelo Milano and Jacob Schroder
Healio/Cardiology Today
First North American patient implanted with next-generation total artificial heart
https://bit.ly/2Ui58G6
July 15 — Carmelo Milano and Jacob Schroder
Yahoo News/Business Wire
CARMAT Announces the First Human Implant of Its Total Artificial Heart in the United States
https://yhoo.it/3rgQURE
July 15 — Duke University Hospital
The Sun
First US-based artificial heart implant for French firm
https://bit.ly/3rpRxsf
July 15 —Carmelo Milano and Jacob Schroder
Health Tech World
CARMAT bioprosthetic heart implanted
https://bit.ly/3Bf0HfG
July 15 — Adrian Hernandez and W. Schuyler Jones
Healio/Cardiology Today
ADAPTABLE points to solutions about aspirin dose, conduct of pragmatic trials
https://bit.ly/3kuhntA
Duke Heart Week Ending July 11th 2021
Highlights of the week:
EXACT Trial Launched; New Gene Therapy Option for Refractory Angina, CAD Patients
EXACT, a first-in-human clinical trial examining the safety and efficacy of using an adenoviral vector to more efficiently deliver human vascular endothelial growth factor (VEGF) directly into the myocardium with the goal of stimulating angiogenesis in patients suffering from refractory angina due to advanced coronary artery disease (CAD), has launched at Duke. Investigators on the trial include E. Magnus Ohman, Thomas Povsic (serving as site and national PI) and cardiothoracic surgeon Adam Williams.



The first treatment at Duke was performed by Williams on June 23.
“This is a very exciting time – this trial is the first of its kind,” said Williams. “It has the potential to change the landscape for patients with refractory angina by providing a new therapy that has the potential to stimulate the body to grow new blood vessels in the heart.”
Patients with refractory angina due to advanced CAD are often referred to as ‘no-option’ patients, according to Ohman.
When patients are first diagnosed with CAD, the treatment approach typically involves lifestyle changes along with medications and, as the disease progresses, interventions such as angioplasty or coronary artery bypass grafting can be performed to improve blood flow throughout the heart. As CAD becomes more severe, however, medications may not be as effective and patients eventually exhaust all options for revascularization. Patients with refractory angina due to CAD have typically had prior interventions to open vessels in the heart, but can continue to experience pain or pressure in their chest due to the diffuse nature of their disease. This is an experience that can be severely debilitating, occurring on a daily basis, significantly limiting their quality of life.
“At this point, Ohman says, “there are very few options and we have been working on trying to figure out more ways to help these patients. This trial represents a significant new option for them.”
Other EXACT trial sites enrolling patients are located in OH, MN, GA and FL.
“Treatments for patients such as these are desperately needed and this is a new option offered here at Duke that is not available elsewhere in this region,” says Povsic. “This option represents a novel approach from conventional revascularization or medical therapy, and aims to address the fundamental deficit of microvascular dysfunction and lack of blood flow to the myocardium.”
According to Williams, most gene therapy trials that have been done in humans use an adeno-associated virus, but EXACT is using an adenoviral vector to deliver VEGF directly into the myocardium. This is done, he says, through a very small, minimally invasive incision to reach the heart tissue. Under direct vision, the surgeon then injects areas of the heart muscle that are known to be ischemic with the goal of stimulating new blood vessel development in that area.
Adenovirus, Williams says, has a quick onset of action – it begins within a couple of days – and after a couple of weeks, it stops expressing the VEGF. The team expects it will take 1 to 2 months post-therapy to start seeing a noticeable difference in the heart tissue.
Importantly, the team will evaluate enrolled patients using positron emission tomography (PET) scans over the course of a year. The scans will provide critical objective data as to whether the intervention is leading to increased blood supply to the ischemic areas.
The team is happy to evaluate any patients who have ongoing angina (chest pain due to coronary artery disease) for inclusion in this or other potential trials. To learn more about the EXACT Trial criteria, please visit: https://clinicaltrials.gov/ct2/show/NCT04125732. To make a referral or discuss a possible patient with a member of the team, please contact the offices of either Dr. Povsic, 919-684-1284, or Dr. Ohman, 919-681-2069, or email Dr. Povsic directly at thomas.povsic@duke.edu.
Pokorney & Duke EP Enroll 1st Patient for Extravascular ICD Trial

Congratulations to electrophysiologist Sean Pokorney and the Duke EP team – they recently became an enrolling site for the Medtronic Extravascular Implantable Cardioverter Defibrillator (EV ICD) Pivotal Study. Pokorney and team did their first implant of the investigational device on Monday, June 14th.
The clinical trial is designed to determine the safety and efficacy of using Medtronic’s investigational EV ICD system to treat patients who are at increased risk of dangerous ventricular rhythms – patients who are at increased risk for sudden cardiac death, who have an ejection fraction of 35 percent or less.
Traditional ICDs are implanted under the skin below the patient’s collarbone with electrode wires (“leads”) placed transvenously, meaning the wires are placed through a vein and into the heart, where they are attached directly into the heart muscle. The location of the leads directly inside blood vessels and heart tissue can increase the risk of blood stream infections in patients.
The EV ICD utilizes extravascular placement, meaning the leads are not placed inside the blood vessels, which eliminates the risk of blood stream infections. The device is the same size as traditional ICDs with a wire that is designed to be placed underneath the sternum and close to the heart without the need for transvenous positioning, according to Pokorney.
“This allows the device to both pace the heart and shock the heart out of ventricular tachycardia,” said Pokorney.
The EV ICD Pivotal Study is a worldwide clinical trial with 50 sites, 23 of which are based in the U.S. Duke is the only enrolling site between Washington, DC and Jacksonville, FL. To learn more about eligibility criteria, please visit: https://clinicaltrials.gov/ct2/show/NCT04060680.
Shout-out to Lindgren!
We received a recognition note this past week about Allison Lindgren, a cardiology PA on 7700. The note was sent to Rio Landa and Faith Williams by Katherine Adams, a clinical team lead for 7700, the cardiology stepdown unit at Duke University Hospital.
“Hi Rio & Faith, I wanted to take a moment to recognize Allison Lindgren. The nursing staff on 7700 submitted a recognition form for Allison for the quality care and team work that she provided from 6/21-6/23/2021. The staff members wrote this on the recognition form:
“Thank you for being someone who we can rely on. You are a great person to work with and we are so lucky to have you as a colleague”
Allison – thank you so much for all of your excellent work on the unit! We really appreciate you!” — Katherine
Way to go, Allison!
ICYMI: Duke Raleigh Hospital Opens New South Pavilion Bed Tower
Duke Raleigh Hospital celebrated the opening of its South Pavilion on Thursday, July 8, with move-in for patients expected to begin on Monday, July 12.
The nearly $196 million dollar project – which includes renovations to the hospital’s existing bed tower — is Duke Health’s largest investment in Wake County to date. The South Pavilion features 92 single-occupancy patient rooms, nine state-of-the-art operating suites and a new kitchen and café for patients and visitors.
“The newly completed South Pavilion adds space, not just for innovative care, but more room for families to be involved in the healing process during their stay,” said Leigh Bleecker, Duke Raleigh Hospital interim president. “This expansion brings us to 256 available beds in our facility — 186 licensed inpatient beds, plus 70 beds for observation and outpatient procedures. This total includes 28 ICU beds — an increase from the 15 we have today.”
The six-story South Pavilion compliments the hospital’s existing North Pavilion, which will be undergoing renovations in August to expand surgical areas, enhance the chapel and create a new corridor to link the two patient towers.
Construction on the new, 210,200-square-foot South Pavilion building began in 2018 and was designed to enhance patient and visitor experiences during their stays. Patient rooms include separate sitting areas for families, and new waiting rooms on inpatient floors overlooking Wake Forest Road.
Additionally, the new building incorporates art throughout, with a large, open lobby displaying work from local artists. The expanded café includes seating for nearly 200 guests and a menu featuring varied cuisines. An outdoor courtyard with dining areas, a tranquility garden and walking paths provides patients and visitors an opportunity to enjoy fresh air and sunshine.
With the new building and renovations in the North Pavilion, Duke Raleigh Hospital will have a new unified front entrance off Wake Forest Road in 2022.
“The building projects at Duke Raleigh Hospital – including construction of the South Pavilion bed tower and the upcoming renovations to the North Pavilion – represent the strength of our commitment to Wake County and the communities we serve,” said William Fulkerson, MD, executive vice president of Duke University Health System. “These projects are designed with careful attention to meeting the health and wellness needs of our patients, visitors and staff — both now and into the future.”
Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged.
Duke Heart in the News:
July 6 — Christopher Granger, Tracy Wang and Manesh Patel
HCP Live
Christopher Granger, MD: Antithrombotic Therapy in Patients with Atrial Fibrillation
https://bit.ly/3qYo0FH
July 6 — Kevin Thomas
Medscape
CABANA: Ablation Bests Drugs for AF in Racial/Ethnic Minorities
https://www.medscape.com/viewarticle/954248
July 7 — Kevin Thomas
Physician’s Weekly
Catheter Ablation May Be Better Option for Non-White AFib Patients
https://bit.ly/2UAk8yQ
July 7 — Stephen Greene and Mohammad Shahzeb Khan
Medpage Today
HF Care in the ED Languishes Despite Congestion-Driven Treatment Strategy
https://www.medpagetoday.com/cardiology/chf/93460
July 7 — Manesh Patel
HCP Live
Manesh Patel, MD: New Therapies for Cardiovascular Risk Management
https://bit.ly/3dXCzEs
July 7 — Schuyler Jones and Tracy Wang
HCP Live
Schuyler Jones, MD: Identifying High Risk Patients for CAD/PAD
https://bit.ly/3woSjXj
July 7 — Kevin Thomas
Reuters Health/MD Alert
Ablation bests drug therapy for minorities with afib in North America
https://bit.ly/3e1RnSC
July 8 — Derek Chew and Duke Clinical Research Institute
Medscape
IV Iron Cost-Effective, Maybe Even Cost-Saving in HF With Iron Deficiency
https://www.medscape.com/viewarticle/954455
July 8 — Kevin Thomas
HealthDay News
Catheter Ablation Improves A-Fib Outcomes in Racial/Ethnic Minorities
https://bit.ly/3AGFgUF
Duke Heart Week – July 4th 2021
Highlights of the week:
Welcome New Cardiology Fellows
This week, we welcomed 10 cardiology fellows to the Duke Cardiovascular Disease fellowship. They are all incredibly talented and have accomplished so much already. We are excited to work with them, get to know them, and watch their careers unfold!
Shown L-R are: Sara Coles; Willard Applefield; Manasi Tannu; Ijeoma Eleazu; Nkiru “Kiki” Osude; Balim Senman; Ilya Shadrin; Lonnie Sullivan; M. Shahzeb Khan, and V. Mark Kittipibul.

Please give them a warm welcome when you see them!
Cardiovascular & Thoracic Surgery Residents, Fellows Celebrated
Congratulations to our incredible residents and fellows who wrapped up their training with us in May:
- Hai Viet-Nguyen Salfity, MD, MPH, Thoracic Surgery Residency Program. She is headed to the University of Cincinnati Medical School, Cincinnati, OH.
- Robert Patrick Davis, MD, Thoracic Surgery Residency Program. He is heading to Yale in New Haven, CT.
- Charles Wojnarski, MD, Thoracic Surgery Residency Program. He is heading to Virginia Mason Hospital in Seattle, WA.
- Eriberto Michel, MD, Thoracic Transplant and Advanced Cardiac Surgery Fellowship. He is headed to Massachusetts General Hospital in Boston, MA.
- John M. Trahanas, MD, Advanced Aortic and Endovascular Surgery Fellowship. He is headed to Vanderbilt Medical School of Medicine in Nashville, TN.
Shown L-R are: E. Michel; J. Trahanas; H. Salfity (front); R. Patrick Davis (rear) and C. Wojnarski; with B. Zwischenberger, associate program director; J. Haney, program director; E. Chen, division chief; B. Tong, associate program director; and P. Smith, former division chief.

We are so excited for you! Best wishes as you embark on the next phase of your careers.
Rao Appointed VISN 6 Cardiology Lead
 We are pleased to share that Sunil V. Rao, professor of medicine in cardiology at Duke and section chief of cardiology at the Durham Veterans Affairs Medical Center, has been appointed as the Cardiology Lead for the VA’s Virtual Integrated Service Network (VISN) 6!
We are pleased to share that Sunil V. Rao, professor of medicine in cardiology at Duke and section chief of cardiology at the Durham Veterans Affairs Medical Center, has been appointed as the Cardiology Lead for the VA’s Virtual Integrated Service Network (VISN) 6!
The Veterans Health Administration is the largest integrated health care system in the U.S. and is comprised of 18 VISNs. VISN 6 is the VA’s Mid-Atlantic Health Care Network, which includes 7 inpatient Veterans Affairs Medical Centers, 7 VA outpatient clinics, and 30 Community-based outpatient clinics in North Carolina and Virginia.
“It is an honor to do this work and it’s a natural progression of the work that all of us at the VA have been doing,” says Rao. “We’ve got a great team at the Durham VA and everyone is interested in increasing the level of care we’re providing.”
Cardiovascular care is a big proportion of the care the VA delivers both on an inpatient and outpatient basis, according to Rao. Because there are a lot of complexities within the scope of cardiovascular services provided, there had become a need to have someone who could serve in a coordinating role in order to improve care delivery to veterans across the VISN.
Rao credits his team at the VA and the strong partnership with Duke as the academic partner for the Durham VAMC, for their ability to provide extraordinary care to veterans.
“We’ve been able to develop treatment pathways – frequently in coordination with Duke –particularly as it relates to the things that the VA just can’t offer, like transplantation and advanced heart care therapies,” says Rao. “To serve as the cardiology lead for the VISN, for me, this is a chance to bring the work that our team at the VA has done and introduce it to a broader audience and try and make cardiology care around the entire VISN more efficient and to increase access to care for veterans.”
According to Rao, he and others within the VISN will be working to identify and address gaps in care for cardiology patients. Their goal is for patients in VISN 6 to get access to the top notch care they need in the places nearest them, and, when necessary, to more efficiently coordinate care with sites in Durham, Richmond or Asheville in the event that more advanced care is needed.
“I think for all of us, it’s really an honor to be able to serve people who have served their country and that is what keeps us dedicated to the VA,” says Rao. “I’m looking forward to seeing how we can elevate the level of care within the VA system both in NC and Virginia. I’m really looking forward to working with the entire team at the VISN level to try and do that.”
Congratulations, Sunil!
Piccini and Duke EP Launch DEFINE AFib Trial with Medtronic
Congratulations to Jon Piccini and the Duke EP team for enrolling one of the first two patients into the DEFINE AFib clinical  trial, a research study funded by Medtronic. Using data collected from Medtronic’s LINQ family of insertable cardiac monitors (ICMs), the study aims to address unanswered questions around atrial fibrillation (AF) burden and its impact on patient outcomes, quality of life, and healthcare utilization. This is the first app-based research study for Medtronic.
trial, a research study funded by Medtronic. Using data collected from Medtronic’s LINQ family of insertable cardiac monitors (ICMs), the study aims to address unanswered questions around atrial fibrillation (AF) burden and its impact on patient outcomes, quality of life, and healthcare utilization. This is the first app-based research study for Medtronic.
Piccini enrolled Duke’s first patient on June 21. A second patient was enrolled the same day at Florida Electrophysiology Associates in Atlantis, FL.
DEFINE AFib will be conducted remotely through the new Medtronic Discovery App in coordination with U.S. sites that will collectively enroll approximately 5,000 patients. Study participants will include patients age 22 or older who have a history of AF, an iPhone device (iOS version 13 or higher), and one of the LINQ family of ICMs, among other criteria. The study will incorporate both device data and patient-reported data derived from scheduled patient surveys and the HealthKit — coupled with electronic health record information about medications and previous cardiac procedures — to provide comprehensive, actionable insights. Through a machine learning approach, aggregated study data will be leveraged to enable improved AF management in the future.
“When it comes to managing atrial fibrillation, there is not a ‘one-size-fits-all’ approach, and the hope is that DEFINE AFib may give us the tools to help personalize AF management based on a patient’s individual health profile and physiology,” said Piccini, associate professor of medicine and director of electrophysiology at Duke, who is also chair of the DEFINE AFib Steering Committee. “DEFINE AFib will harness the power of digital health to make fundamental discoveries about how we can manage atrial fibrillation better in each and every one of our patients.”
Congratulations, Jon and team!
Shout-out to DeVore & Karra
We received the following note this week from our anesthesiology colleague Yuriy Bronshteyn:
“Hi, I’m an intensivist-anesthesiologist here at Duke and wanted to recognize two of your faculty for their dedication and patient-centric care:
- Adam DeVore
- Ravi Karra


Last week, a patient who lives 4+ hours away came to our anesthesia pre-op clinic anticipating surgery the next day for a slow-growing cancer. Unfortunately, her EKG showed some concerning findings so her surgeon asked that the cancer surgery by postponed pending a cardiology evaluation. The patient was distraught and asked only that her cardiology workup happen at Duke the next day since she was already staying at a local hotel overnight and that she would have difficulty returning to Duke later. At 5:30 p.m., Dr. DeVore – while wrapping up a busy clinic day – personally scoured the cardiology schedules and found a slot for the patient the next day with Dr. Karra. Dr. Karra then generously agreed to see the patient and proceeded to take excellent care of her.
Dr. DeVore and Dr. Karra went above and beyond to help a patient who was at risk of falling through the cracks of the healthcare system. And at a time when the patient was dealing with the emotional consequences of a cancelled cancer surgery. It is acts like this that make Duke an exceptional place to work and receive care.
Thank you to Dr. DeVore and Dr. Karra!” — Yuriy
We agree! Nicely done, Adam and Ravi!
Have news to share?
If you have news to share with the Pulse readership, please contact Tracey Koepke, director of communications for Duke Heart at tracey.koepke@duke.edu. We would love to hear about your latest accomplishments, professional news, cool happenings, and any events or opportunities that may be of interest to our Duke Heart family. Please call with any questions: 919-681-2868. Feedback on Pulse is welcome and encouraged.
Duke Heart in the News:
June 29 — L. Kristin Newby
Mirage News
https://bit.ly/3hkTL7K
June 29 — Raymond Kim
Diagnostic Imaging
Cardiac MRI Picks Up Myocarditis in Patients Fully Vaccinated for COVID-19
https://bit.ly/2TwVv5S
June 30 — Susan Dent (medical oncology)
Health Day
https://bit.ly/3hvnoDs
June 30 — Keisha Bentley-Edwards (internal medicine)
Triangle Tribune
‘Denomination matters’ in Black-focused faith-based health programs
https://bit.ly/3qRO3i4
July 1 — Han Kim
Physician’s Weekly
Covid-19: New Reports of Vaccine Linked Myocarditis
https://bit.ly/2V40Thk
Division of Cardiology Publications Indexed in PubMed June 24-30, 2021
Curtis LH, Hoffman MN, Califf RM, Hammill BG. Life expectancy and voting patterns in the 2020 U.S. presidential election. SSM Popul Health 2021;15:100840. PM: 34169139.
Hamo CE, Abdelmoneim SS, Han SY, Chandy E, Muntean C, Khan SA, Sunkesula P, Meykler M, Ramachandran V, Rosenberg E, Klem I, Sacchi TJ, Heitner JF. OUTpatient intravenous LASix Trial in reducing hospitalization for acute decompensated heart failure (OUTLAST). PLoS One 2021;16(6):e0253014. PM: 34170908.
Hoffmann U, Lu MT, Foldyna B, Zanni MV, Karady J, Taron J, Zhai BK, Burdo T, Fitch KV, Kileel EM, Williams K, Fichtenbaum CJ, Overton ET, Malvestutto C, Aberg J, Currier J, Sponseller CA, Melbourne K, Floris-Moore M, Van Dam C, Keefer MC, Koletar SL, et al. Assessment of Coronary Artery Disease With Computed Tomography Angiography and Inflammatory and Immune Activation Biomarkers Among Adults With HIV Eligible for Primary Cardiovascular Prevention. JAMA Netw Open 2021;4(6):e2114923. PM: 34185068.
Lopes RD, de Barros E Silva PGM, Furtado RHM, Macedo AVS, Ramacciotti E, Damini LP, Bronhara B, Cavalcanti AB, Rosa RG, Azevedo LCP, Veiga VC, Machado FR, Ritt LE, Martins PA, Alexander JH, Avezum A, Berwanger O, et al. Randomized clinical trial to evaluate a routine full anticoagulation Strategy in Patients with Coronavirus Infection (SARS-CoV2) admitted to hospital: Rationale and design of the ACTION (AntiCoagulaTlon cOroNavirus)-Coalition IV trial. Am Heart J 2021;238:1-11. PM: 33891907.
Malian HM, Smith PJ, Hoffman B, Jiang W, Ammerman K, Kraus WE, Hinderliter A, Sherwood A, Blumenthal JA. Effects of Acute Exercise on Anxiety Ratings in Patients With Coronary Heart Disease and Elevated Anxiety. J Cardiopulm Rehabil Prev 2021;41(4):277-281. PM: 34158457.
Singh H, Mehta RH, O’Neill W, Kapur NK, Lalonde T, Ohman M, Ghiu I, Chen-Hsing Y, Dutcheshen K, Schreiber T, Rosman H, Kaki A. Clinical features and outcomes in patients with cardiogenic shock complicating acute myocardial infarction: early vs recent experience with impella. Am Heart J 2021;238:66-74. PM: 33848505.
Vogel RF, Delewi R, Angiolillo DJ, Wilschut JM, Lemmert ME, Diletti R, van Vliet R, van der Waarden NWPL, Nuis RJ, Paradies V, Alexopoulos D, Zijlstra F, Montalescot G, Krucoff MW, van Mieghem NM, Smits PC, Vlachojannis GJ. Pharmacodynamic Effects of Pre-Hospital Administered Crushed Prasugrel in Patients With ST-Segment Elevation Myocardial Infarction. JACC Cardiovasc Interv 2021;14(12):1323-1333. PM: 34167672.
Recent Comments