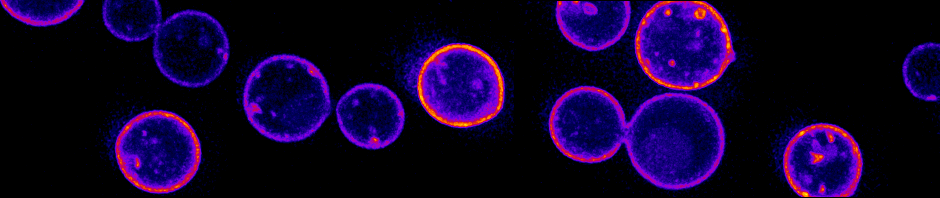
In order to cause human infections, microorganisms must be able to adapt to the hostile environment of the infected host. For example, one of the fungi that we study in the laboratory, Cryptococcus neoformans, creates a large surface capsule to avoid the host immune system. Capsule is highly expressed in the setting of infection, and minimally expressed when the fungus grows in the test tube. We are interested in determining how infectious microorganisms sense the host and respond with these types of protective cellular responses. In this way, we hope to identify new targets for treating infectious diseases.
Our laboratory primarily uses the tools of fungal genetics to study the pathogenic process. Fungal pathogens have become increasingly important in immunocompromised patients, especially those with HIV infection or organ transplantation. By defining and manipulating gene expression patterns in these microorganisms, we are able to assign function to specific gene products. By looking at global genome expression patterns, we are finding new genes and gene families that are important for microbial pathogenesis.