Patient Story
The Eddys

The spine is a common site for cancer to metastasize (spread). In fact, research shows that between 30 and 70 percent of people with metastatic cancer will experience a tumor on their spine.
Unfortunately, it is also common for people to be unaware that they have any cancer at all until it has spread from the primary site – perhaps the lung or breast — to the spine.
This was the case for Chad Eddy of Wake County, NC, who was feeling fine until a nagging back pain started. His X-rays looked normal, so he tried physical therapy. The pain only got worse, until he was at times unable to walk. Finally, an MRI showed masses on his spine and a broken vertebra.

Follow-up appointments were scheduled, which would not be kept. Chad explains: “I woke up one morning and a voice in my head screamed, “GET YOURSELF TO A HOSPITAL NOW.” He and his wife, Missy, called for an ambulance, and asked the paramedics to take him to Duke. “Suddenly, I felt like I was going to be taken care of,” he says. “I had never been to Duke, but I knew that it had a national reputation.”
At the emergency department at Duke University Hospital, Missy gave Chad’s MRI scans to Michael O’Keefe, MD, an emergency medicine physician. Chad remembers O’Keefe telling him, “We have a neurosurgeon upstairs, we’re connected to the top people, and we’re going to work fast on this.” Chad and Missy felt relief. “That was the first time anyone said we’re going to move fast,” says Chad. As they mentally prepared to face surgery the next day, they were shocked once again to learn it would happen in just three hours.

Duke neurosurgeon Rory Goodwin, MD, PhD, was on call when Chad and Missy arrived at the ED. Goodwin is co-leader of the new Duke Center for Brain and Spine Metastasis and specializes in treating tumors of the spine.
Chad said Goodwin immediately put him at ease. “He walked in and told me not to worry, that they were going to do what they needed to,” says Chad. “His confidence was so comforting.” Missy felt the same. “If there’s one person you want on your team, it’s him,” she says.
In a six-hour surgery, Goodwin removed the tumor and performed a spinal fusion by placing a cage between two vertebrae. It was after the surgery that Chad and Missy got the diagnosis: He had stage 4 non-small cell lung cancer, caused by an EGFR mutation, that had spread to his spine.
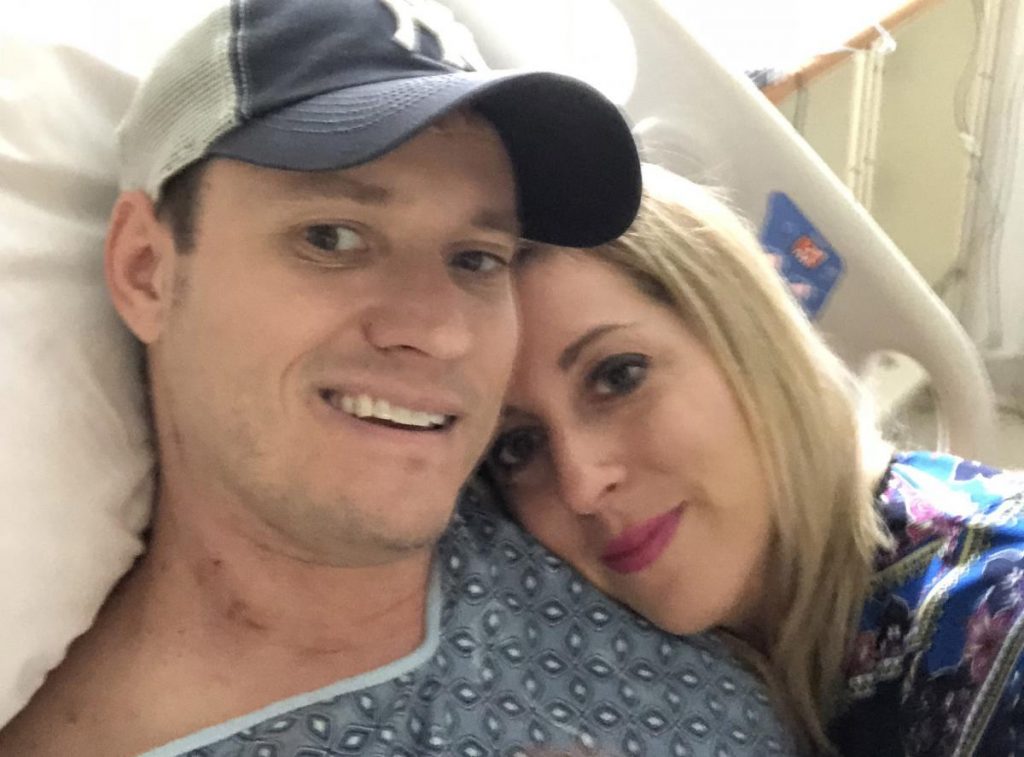
A few days after surgery, Chad was up and walking, determined to start down the road to recovery. The surgery was followed by targeted therapy (osimertinib) and radiation treatments. Meanwhile, Chad, a former athlete, went from walking to running for short intervals. He and Missy never stopped living their lives. “Six weeks after the surgery, I packed him up and took him to the beach,” says Missy.
His last scan, six months after surgery, showed one small spot left on his lung.
“God blessed our family and worked some miracles through the skilled professionals at Duke,” says Chad. “We’ve learned to appreciate life at a new level, and we’ve learned that we have to be vulnerable and allow people to help. When we got to Duke, I was able to let go.”
Katie Mackin

In November 2017, Katie Mackin was a 34-year-old mother of a six-month-old baby when she felt something in her back pop. Mackin is a physician assistant in an orthopedic practice, and her first thought was that she had a slipped disc. The pain kept getting worse, even after two months of physical therapy and anti-inflammatories. In January 2018, an MRI revealed tumors on her spine, which turned out to be metastases of breast cancer that Mackin didn’t know she had. By February, she was having spine surgery at the Duke’s Center for Brain and Spine Metastasis.
Fast forward to March 2020. Mackin missed only about five months of work, and is able to keep up with her two-and-a-half year old son. “I’m able to do most of the things I want to do,” she says. And she attributes that to the care she’s gotten from providers at the Duke Cancer Center, including spine surgeon Rory Goodwin, MD, PhD.
“He has been fantastic,” she says. “I can’t say enough good about him. He makes you feel like you’re a person, not just another patient-number.”
When Mackin first met with Goodwin, he explained that surgery to remove cancer and stabilize her spine carried a risk of paralysis, but doing nothing carried a higher risk of paralysis. “It was a no-brainer,” she says. “I felt super confident with him. He had every scenario covered.” The surgery went well, and Mackin started back at work, part-time at first, just five months later.
Mackin had radiation before surgery for pain relief in her hip and lower back, with the goal of making post-surgical rehab easier. She also started on Trastuzumab (Herceptin) and Pertuzumab (Perjeta), which she continues to this day, at three-week intervals. After the surgery, and more radiation to kill any remaining cancer cells, she also underwent several rounds of chemotherapy.
Since then, she’s done well. “When you’re stage 4, you never get told you’re in remission,” she says. “But I’ve been stable since August 2018, and I hope to be stable for a lot longer.”